- Home
- Charcot foot
Quick Summary: Understanding Charcot Foot
- What it is: A serious condition where bones in the foot weaken and fracture, often leading to severe deformity.
- The Main Cause: Most commonly triggered by diabetes and peripheral neuropathy (loss of sensation).
- The Warning Signs: Look for swelling, redness, and heat in one foot—even if there is no pain.
- Urgency: Early detection is vital. Untreated Charcot foot can lead to permanent disability or amputation.
- Primary Treatment: Immobilization through total contact casting to allow bones to heal without further collapse.
Charcot foot
Author: Dr. Marc Mitnick
Reviewed by: Medical Review Board
Charcot osteoarthropathy or neuropathic joint disease
WHAT IS CHARCOT FOOT
This condition, also known as charcot osteoarthropathy or neuropathic joint disease is a chronic, progressive and destructive process that affects the bones and joints of the foot.
CHARCOT FOOT CAUSES
Jean-Martin Charcot was a French neurologist who in 1868 first recognized the association between neurological disease and the resulting bone and joint destruction in the lower extremities. During this period the relationship was between tabes dorsalis (neurosyphillis) and the destruction to the joints in the feet.
Today, in the industrialized world diabetes is the number one cause of Charcot foot.
Other causes include:
- alcoholic neuropathy
- cerebral palsy
- leprosy
- multiple sclerosis
- rheumatoid arthritis
- pernicious anemia
- lyme disease
- spinal cord injury
The problem is due to lack of proprioception, the inability to ‘feel’ the ground that you are walking on. A good example of proprioception is seen when walking on a rocky terrain such as a gravel driveway. As your foot comes down on a rock sticking out of the ground, your brain recognizes the fact that the foot is not going to come down properly on the ground (due to the rock) and you are able to make adjustments in order to keep walking forward.
With any neuropathy (loss of sensation to the feet), the connection is not made between the feet and the brain, the feet do not adjust properly and there then becomes excessive strain placed on the joints and bones of the foot. Over time these joints and bones begin to break down.
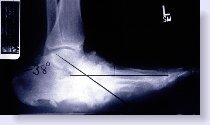
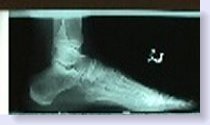
Below is an x-ray of a Charcot foot deformity on the left. Compare it with the x-ray of a normal foot on the right. The pathological changes should be apparent even to the untrained eye. Note the loss of the arch and all the bone destruction that has occurred where the arch was once located.
|
|
STAGES OF CHARCOT FOOT PROGRESSION
The Charcot foot disease process is generally broken down into three stages.
Stage 1: The Acute Destructive Stage
- Clinical Signs: Characterized by profound swelling, increased skin temperature, and redness. This is caused by increased circulation and often mimics a localized infection.
- X-Ray Findings: Initial x-rays may be negative, but more commonly show soft tissue edema, joint effusion (swelling within the joints), and joint subluxation (misalignment).
- Physical Paradox: Despite bone fractures and fragmentation occurring internally, the foot may not be painful due to neuropathy.
- Critical Window: This is the most vital stage for medical intervention; the earlier treatment starts, the less permanent damage occurs.
Stage 2: The Sub-Acute Stage
- Signs of Healing: Marked by a reduction in edema (swelling), temperature, and redness.
- Fragment Absorption: During this phase, the body begins to absorb bone and cartilage fragments.
- Consolidation: Existing fractures begin the active healing process.
Stage 3: The Chronic Stage
- Remodeling: The body attempts to stabilize the foot and restore bone function through remodeling.
- Permanent Damage: While the body is trying to stabilize, the structural damage at this point is usually already permanent.
- Goal: Focus shifts from managing inflammation to stabilizing the resulting foot shape to prevent future ulcers.
Charcot foot fracture and ulcer
The ‘damage done’ consists of a foot that no longer functions in a normal gait cycle. Because of the abnormal shape of the foot due to breakdown and fracture, there is usually excessive pressure points on the skin that will eventually breakdown and ulcerate out. (see my discussion on the diabetic foot and Charcot disease.) Since an ulcer is an opening in the foot it is subject to infection.
Even if it does not become infected, the ulcer itself can take months, if not years, to finally close. If it does become infected you risk invasion of the bacteria into the bone resulting in an osteomyelitis (bone infection) and possible amputation. Because Charcot foot is seen more so in patients with neuropathy, elevated blood sugars and usually poor circulation it is not uncommon for the above scenario to play out.
CHARCOT FOOT PREVENTION
Early detection and treatment is the key to avoiding excessive damage. A common theme of mine in this site is for diabetics to have a proactive approach in the care of their disease, meaning, making all efforts to control their blood sugar, because even though you may feel fine, if your blood sugars are continually elevated you are doing damage to yourself on a daily basis.
Inspecting your feet regularly. In the case of suspected Charcot foot, should you notice a difference between your two feet, (as this condition usually only occurs in one foot) such as one foot is more swollen, warmer to touch or more red than the other foot, this should be brought to the immediate attention of your doctor.
regular medical check ups from both your medical doctor and podiatrist.
Charcot foot orthotics wearing a good orthotic on a regular basis goes a long way to prevent the slow, gradual breakdown of the joints in the foot.
CHARCOT FOOT TREATMENT
CASTING AND IMMOBILIZATION Treatment consists of immobilization and if possible non-weightbearing on the affected foot in an effort to curtail any further destruction. We use what is known as a total contact cast which is cast or boot that is molded to the bottom of the foot to provide even distribution of body weight over the entire bottom of the foot and therefore to create even pressure on the foot to prevent further breakdown.
Depending on the acuteness of the stage and other factors such as inadequate blood sugar control, obesity and patient compliance, total contact casting may be necessary any where from six weeks to several months.
In addition to immobilization a class of drugs known as biphosphanites (Pamidronate) are being used intravenously to help heal the bone fractures that occur. Medication would be used during the first two phases of the disease.
BONE STIMULATORS In addition to medication, there has been some experimentation with bone stimulators to also heal the pathological fractures that occur. This would also be indicated during the first two phases of Charcot foot.
MOLDED SHOES Treatment for the end result of the damage done usually requires special shoes that are molded to the newly deformed foot in an effort to protect bony protrusions and to prevent further breakdown. Even though the inflammatory part of the disease has diminished, we now are left with a poorly functioning foot which in itself is subject to further breakdown.
SURGERY If there are parts of the foot that are left severely deformed many times surgical intervention will be indicated in an effort to remove any excess bony prominences and to fuse any weakened joints to prevent further degradation of the foot. Most of the resulting problems are located on the bottom of the foot.
FREQUENTLY ASKED QUESTIONS
What are the first signs of Charcot foot?
The earliest signs (Stage 1) include profound swelling, increased redness, and a noticeable increase in skin temperature. These symptoms often mimic an infection but are actually caused by increased circulation and bone fragmentation.
Is Charcot foot painful?
Surprisingly, Charcot foot is often not painful. Because the condition is typically caused by neuropathy (nerve damage), patients may not feel the fractures or joint destruction occurring internally, which often leads to dangerous delays in seeking treatment.
Can Charcot foot be cured?
While the inflammatory process can be stopped and the foot stabilized through casting and immobilization, the structural damage and bone deformities are usually permanent. Treatment focuses on preventing ulcers and further bone breakdown.
What is the main cause of Charcot foot?
In the industrialized world, diabetes is the leading cause. It results from a combination of loss of sensation (proprioception) and adequate blood flow that allows the bones to wash out and weaken.
How long does treatment take?
Depending on the severity and stage, total contact casting and immobilization may be necessary anywhere from six weeks to several months to ensure the bones have properly consolidated.
REFERENCES
If you happen to live in the New York - New Jersey area and would like to visit our office
|
|
To make an appointment online or for directions to our office click Dr. Marc Mitnick.
DISCLAIMER: The purpose of this site is purely informational in nature. It is not intended to diagnose, treat or cure any medical condition. This information is not a substitute for advice from a medical professional. Please consult your healthcare provider for accurate diagnosis and treatment. The information presented here may be subject to errors and omissions.
SITE LAST UPDATED: MAY 2026


I've been doing some aggressive research lately (it's how I found your incredible website) and realize now that my symptoms are not consistant with the diagnosis.
Jennifer
Hunterville, NC
….after reviewing your amazing site (great for the avg. jill). So thank you very much!!!
Liesbeth
NY
I am really, really impressed with your plain-speak explanations for the various conditions.
Jacqueline
NJ
This was an extremely helpful site. I have an appointment on the 18th and your info. Was right on target…..
Jack
Fla
A well organized site containing much information written in a manner that the average reader can comprehend.
Jean
Ontario, Canada
I found your website and articles most interesting.
Andrew
Fla.
Thank you for a quick response. I think your site is the best information site on foot pain and I have viewed many.
Judy
(location unknown)
I came to your website, footspecialist.net via www.foot-pain explained .com which I think is also your website? I thought explanations for different types of problems were well addressed and thoughtfully stated for the patient in mind.
L.W.
New York
You have an amazing and extremely informative site. I enjoyed looking through all of the data and stats.
Yvette
Memphis, TN
Thanks again so much for the information in the article. Very interesting.
Anna
Scotland
Great article. I have had plantar fasciitis since I was in high school……..
J. Simmons
(location unknown)
Dear Dr. Mitnick, The orthotics arrived four days ago and I slipped them into my shoes immediately. I was skeptical as to the usefulness of the item, they really didn't look very exotic. I have to say though, after using them for just four days, I have experienced grand relief from my foot pain. Even the very first day, I was able to do a lot of work while on my feet with at least a 75% reduction of pain. It has only gotten better every day, and I go nowhere without my shoes with the orthotics. I had been experiencing extreme heel and sole pain for about six months and had to take extended breaks off my feet many times a day as well as regular doses of Ibuprofen. Since getting the orthotics, my life has returned to normal and I feel good again. Just wanted to say thanks for the recommendation for a very effective item, I had no idea what a change this item could affect.
Yours truly,
J.C. Forbes
Tennessee
Thanks for the Response, you hit it on the head.
Steve
Redondo Beach, CA
Thank you for your time and expertise in answering my question…..
LH
(location unknown)
First, thanks for putting together this website. Its the most informative site I have found dealing with foot problems. Last June I started having pain and swelling at …….
Joe
(location unknown)
First of all, thank you for having all this useful information available in one place. I've been through most of your website and based on my research, pain and evaluations I think I've narrowed things down quite a bit.
Pete M.
(location unknown)
Thank you for the best site I have found when researching foot pain.
Glenda B.
Madison, Alabama
Thanks for replying so quickly. I was a bit concerned. I think your website is great, and chock full of info.....
Carol
Denison, TX
Dr. Marc, Thank you so much for your reply which seemed to be right on. I have researched many sites but you put me on the right path to the possible answer. My foot pain may not rule the rest of my life after all! I believe I'll make a sign that reads, "THE END IS NEAR!" Thanks Very Much,
Dawn
West lafayette, IN
Dear sir...no doubt you get positive comments re your site...May I please be added to the list of your admirers. In all of my years of web surfing I would say your site is right there with the very best. Thank you for taking the time to write the terrific info you provide and for putting things into laymen terms for us mere mortals. I pray you have much on going success and thank you again for a deed well done. As for me I did not find much help for my symptoms and will continue on my quest. Were you anywhere in the South I would make and appointment...Thanks again dear sir...m.e.
Michael E.
Tampa, Florida 33624
Hi. This is a great site! I'm a healthy middle aged woman who is in good health, but.....
Kelly
Texas
Just a wee word of thanks for your wonderful website...It is a terrific service...Thank you for providing your knowledge and help...With highest regards, m ebeling
Michael D. Ebeling
Tampa, Florida 33624
Thanks for a most interesting website, which has helped a lot.
Steve
UK
Dear Dr.Mitnick
I usually do my research on the Mayo clinic website. I think your website is the most informative site I have found when researching foot pain.
I thank you for putting together this incredible website.
Regards,
Dragica W.
Edmonton,Canada
....I have been told that it is not hard enough to be cut off. Please help, I am not sure what to do now! THANKS FOR A WONDERFUL AND VERY HELPFUL SITE!
Roxy
South Africa
You have an unusually clear, informative and well-written website for laypersons. Thank you for that.
Matthew W.
Mansfield Ctr, CT
First, I'd like to thank you for all the information that you provide on your website and the opportunity to write to you.
Steve
Placentia, California
First, I want to let you know that you have the best web site I've found related to foot issues. (The only thing I had difficulty finding was the "ask a question" page.)
Unknown
Unknown location
I received the orthotics Monday afternoon and began wearing them Tuesday. After two days I would say that I have noticed a huge improvement in the discomfort I have been experiencing. My foot feels better than it has in months.
Ric J.
Unknown location
I greatly admire someone like you who would donate and dedicate so much time and effort to helping strangers with no compensation. Truly, it is uncommonly kind. And your site is so intelligently arranged.
Ron R.
Pacific Grove, CA
I used to work for a podiatrist (front desk) back during summers in college years ago, so I know the benefits of good care. Again, I want to thank you for an EXCELLENT website. It was so great to get to your site (top of google search) and actually find all the answers I needed EASILY and QUICKLY! Clearly you put a ton of work into it and I really appreciate it.
All the best,
Victoria
Alameda, California
By the way, millions of websites could use yours as a guideline on how to organize information and make the site user-friendly. Kudos to you!
Anonymous
Thank you for your very interesting and informative site!
Anonymous
Hi. I come to your site often looking for information. It is really informative and I appreciate it very much. I have RA and have been having considerable amount of foot pain...... Dee RN
Thanks very much for the wonderful informative site.
Catherine
New Zealand
Thank You for my answer! I have been schedule for a bone density scan, allingment, and I am in the process of getting orthotics made, and checking out the natural remedies. Thank again! What a great web site!
Sincerely
Josette
Yes I want both pair of orthotics. You don't have an option of ordering 2 at one time so I had to place the order twice. Thanks. My husband likes these and wants to put them in all of his shoes. (referring to Superstep orthotics)
Cindy H.
Arizona
I searched the internet everywhere for a clear description and illustration of my symptoms/problem. https://www.foot-pain-explained.com/ was where I ended my search with answers. If I lived in Jersey (left 30 years ago) and didn't live in Florida I would definetly make an appointment with Dr. Mitnick.
Thanks, Kathy
Florida
1st of all THANKS A LOT for your great site......
Anna
Poland
Thank you so much for your response. I will let you know how I am doing if you would like. Your website is awesome!
M P
South Carolina
Hello! I want to thank you for such an informative website! I found you based on my ankle pain search and am happy to realize that there may be a relatively simple cause and solution....
Natalie
unknown location
...Thanks for your fantastic service.
Gary
Arlington, VA
Thank you so very much, that would be much appreciated. I love those insoles, by the way. (referring to Superstep orthotics)
Kelly W.
San Clemente, CA
Dr Marc is fantastic...He seems to know exactly what you are feeling with the problems you are having. I wish he was in my home town so I could go to him with my problems!!!!!!!!!!!!!
Pam
location unknown
Great insights! Thanks Doc, you're the best.
Glen
location unknown
I have been experiencing foot pain of various sorts and am working to figure out what it is. I found this site and can only say BRAVO!! What an excellent site! The time it must have taken to put all this together must've been a daunting task! I am sure it has helped so many people. Thank you so very much for doing this.
Bre
location unknown
Dr. Mitnick, Thank you so much for your reply. I did let my physician know and they took an x-ray - all is well! Also, thank you for providing this wonderful site, it is very helpful with lots of useful information! I appreciate your gift of time! God bless.
anonymous
Dr. Mitnick, Thank you, you were 100% correct. The pain finally brought me to the ER. I spent 8 days in the hospital. The Doppler you spoke of was able to show that there was no pulse in that foot. This was an arterial clot that split and traveled throughout my leg. My leg was almost amputated. I am in rough shape but have all my parts intact!! You certainly know what you are talking about. Thank you for taking the time to answer. Yours Truly!
anonymous
Staying at home after hallux surgery I spend quite a lot of time seaching info useful for avoiding problems which might come back. Today I found your site and I am .... delighted it happened. It's one of the best site I found last days.
Anna
Poland
Thanks for taking time to read and answer so many questions. It is truly a public service!
Esh
Seattle, WA
I just wanted to say that I am very greatful for this website!!
Bonnie
location unknown
Also, and importantly, just want to praise this web site. Thorough and thoughtfully presented, it certainly must be of considerable assistance to anyone with a foot problem. Terrific -- and very interesting.I trust the address comes up easily for those seeking information.
Bill
New Jersey
Thanks so much for answering my question. You've been more help to me than my own Dr. has been lately. Thanks again....I hope to be able to walk without pain someday.
Debbie
location unknown
Wow, that is exactly the information needed!!! thank you thank you thank you!!! I appreciate this help so very much from Marc Mitnick DPM. Excellent information and help to improve One's life.
Chrissy
location unknown
Thanks so much for this website Dr. Marc! It is so nice that you have this ask the doctor feature..I'm sure I'ts been helpful for alot of people. I will try what you suggested and see if it helps...thanks again!
Tracy
Evansville, IA
Dear Marc
I just want to say thank you for the quick response and the good info. I find it amazing and a super nice thing that you do here by answering medical questions at no charge.
Russ W.
location unknown
Your website is full of a lot of helpful information, and I am very impressed with the time in which you responded to my post. Thank you again for your time and consideration in your response.
-Sunny.
location unknown
Thank you very much for the information, I will consider it. Excellent web site.
Jackie
San Diego, CA
Dr. Mitnick, Just want to say thank you so very much for your quick response and very informative reply! After reading what you had to say, I called the doctor's office and was able to get in and see him the same day as my injury. Toe was x-rayed and luckily, it is not broken or fractured. Very badly bruised and will probably lose the toe nail. And although my toe and toe nail are still very black and blue and very sore, they ARE both starting to feel a little better. So again, thank you! I am so very happy that I came across your website. The service you provide is outstanding and immeasurable!
Rivi,
Albany, NY
Thank you so much for all of your advice. In searching the web for people dealing with this same issue i can tell you that you are a Knight In shining Armor! If I lived in Jersey I would gladly be your Spokesperson. Hopefully next time you hear from me it will be good news. God Bless,
Jill S.
location unknown
THANK YOU SO VERY MUCH FOR YOUR TIME AND EFFORTS, YOU ARE SO VERY APPRECIATED. THANK YOU FOR ALL YOU DO.
Jackie
Whichita, KS
thanks again, this site is very helpful.
mark
Boston, MA
Like others have stated...This site is amazing and I am so thankful that it was created.
....Keep up what your doing. Your a life saver.
Michelle
Colorado
Thanks again for the information provided on your site. It's easy for non-medical folk to understand your writing, and helps provide better communication between patient and doctor.
annielou
Colorado
Wonderful advice
by: Anonymous
This is the best site for foot problem info.
Thank you for this information. This description fits my pain and inflammation behind my 2nd toe perfectly.
by: Max
location unknown
Again, I really appreciate that you responded to my inquiry, and that your mention of Parkinson's helped me to find my way to a diagnosis of this difficult to diagnose disease. Most patients see on average 16 doctors before they are diagnosed. I hope that you can help other people that ask for your expertise in the future.
Barb D.
Canada
I just wanted to say that I am very greatful for this website!! I have had a fusion in my rt foot and am finally getting a little bit better......
Bonnie
location unknown
Again, Thank you from the bottom of my heart for taking the time to answer my question....your an angel!
Nancie
Wisconsin
Thank you for your response. You have provided some great insight (to my question)....
Julie
location unknown
Thank-you so very much for responding so quickly and in such detail to my question!! I will give my surgeon a call today!! This website is terrific!!!! Thank-you again!
Renae
North Carolina
Many Thanks Dr Marc!
Thank you for your response. It sounds like a good plan to me. He did not cut the wart out first ...
KG
location unknown
Thanks again doc for having this website and we STILL need qualified Podiatrists in beautiful sunny Tampa Bay (Bradenton) Florida.
Bessie Mae
Florida
Dear Dr. Mitnick, Thank you so very much for taking your time to answer my question. You have greatly relieved my anxiety related to the continual tingly I feel in my feet. I will share your response with my podiatrist next week. God bless you for having this question and answer page on your website! Most gratefully,
Lynne T.
location unknown
Your webpage is excellent, I commend you on sharing your knowledge to the public.
Robert
New Jersey
Thank you. you were more detailed than what others have told me they finally called from the last xrays and my son is now in a cast for 2 weeks he did have a fracture that was not noticeable.
a mom
location unknown
I have read your website and I have to admit that I am amazed at all the information that is on here. I have learned more than the three years I have been going to several doctors that I have seen!!
Melody
Lenoir, NC
Thank you so much Doc for a quick and thorough response!
Rustam
Bellevue, WA
I cannot thank you enough for your response, opinion, and suggestions! I want you to know how much it means to me, and I'm sure everyone else who has ever asked you a question! I feel like you're a lifesaver and have empowered me to take a stronger role and stand up for myself and my feet!
Jodi
location unknown
Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…