- Home
- bunion
Quick Summary: Understanding Bunions (Hallux Valgus)
- What it is: A progressive deformity of the big toe joint, characterized by a bony bump (hyperostosis) on the inside of the foot.
- Primary Cause: While footwear can aggravate the condition, the root cause is typically inherited foot structure and poor biomechanics, such as excessive pronation.
- Key Symptoms: Pain from an inflamed bursal sac, joint stiffness due to cartilage erosion, and the big toe deviating toward the second toe.
- Non-Surgical Options: Use of custom orthotics to improve alignment, wide-toed footwear, and night splints to maintain toe position.
- Surgical Correction: Recommended when pain affects daily quality of life. Modern options include Lapiplasty 3D correction, Austin bunionectomy, and TightRope fixation.
bunions
Author: Dr. Marc MitnickReviewed by: Medical Review Board
hallux valgus and tailors bunion
WHAT DOES A BUNION LOOK LIKE
Otherwise known as hallux valgus, this is a deformity of the big toe joint. This type of pathology is usually manifested as a bump on the inside of the foot just behind the big toe. The bump can be very small or reasonably large; the size of which is not necessarily proportional to the amount of pain one can experience.
Along with this bony bump there can be an associated bursitis which is a “cushion” that the body originally creates to protect an area from pressure or friction, but after a while this cushion can also become inflamed and painful.
The last component of this deformity is the deviation of the big toe as it moves toward the second toe, sometimes even underlapping or overlapping the second toe.
Here is a skeletal representation of a big toe joint deformity on the left, compared to a normal foot on the right.

|
What does a bunion look like? Below is a hallux valgus deformity (blue arrow) with the big toe under lapping the second toe.
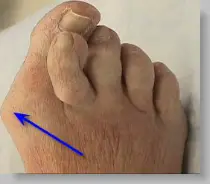
|
WHAT CAUSES BUNIONS
Poor fitting and high style shoes are usually blamed as the culprit for the formation of this deformity, that is why they are more prevalent in women.
But, is that really what causes bunions?
Inherited foot structure-The truth is most of these deformities are based on a particular foot structure and the way a person walks. This is one of the reasons you can see this development in children who typically wear very conservative shoes.
The biomechanics behind hallux valgus formation-The short story is feet that have a tendency to excessively pronate cause an over-flattening of the foot.
- This excessive flattening causes excessive tension on the extensor hallucis longus tendon (the tendon on the top of the foot that enables you to bend your big toe upwards).
- This causes the tendon to "bowstring".
- In doing so forces the big toe to be pulled laterally, toward the second toe. This is what causes the initial deviation.
- Over time, there is a retrograde (or backward) force placed on the first metatarsal bone by the big toe.
- The first metatarsal bone begins to move medially (or away from the second metatarsal bone).
- Due to these changes there is now more pressure on the side of first metatarsal bone from shoe pressure and this causes a hyperostosis or thickening of bone and this results in the bump, that you see and feel on the inside of the foot.
This deformity also creates an unequal alignment of the joint itself and causes the joint to wear out, over time. Once the joint is worn down sufficiently pain ensues when you try to bend the toe while walking.
So, the biomechanics of the foot is really what causes bunions.
In theory, if you lived on a tropical island and never wore shoes your whole life, you could still develop hallux valgus.
Below is a video describing what causes bunions in technical detail.
Generally speaking, hallux valgus is a progressive deformity and in most people will worsen over time (if appropriate measures are not taken to remove the underlying cause).
SYMPTOMS OF A PAINFUL BUNION
- BURSITIS-The most common pain associated with hallux valgus is the pain that occurs from the inflamed bursal sac, also known as an inflamed bunion. Typically, there will be a burning sensation in that area of the foot. Inspection will reveal swelling and redness. This can occur even with very small bumps on the side of the foot. Shoes, particularly women's dress shoes create a lot of pressure against the bone and the body's reaction to that is to form a bursal sac which initially is designed to protect the area, but invariably, will become inflamed and begin to hurt. Whenever, I do bunion surgery, I always look for, and have removed inflamed bursal sacs.
- BUMP PAIN-Even without a bursitis, the bony bump can become painful, again usually aggravated by dress shoes, but in many individuals, even conservative shoes like sneakers will cause pain. The size of the bump and the activity level of the patient are two factors that will lead to bump pain. In this instance there does not necessarily have to be swelling and redness. This pain is usually only evident when wearing shoes and will vary with the type of shoe being worn.
- JOINT PAIN-The other type of pain in this condition is what is known as joint pain. As the big toe starts to move closer to the second toe it creates an abnormal alignment in the big toe joint. This causes a premature erosion of cartilage and over time the joint will no longer move smoothly and the patient will start to experience pain and limitation of motion of the big toe. This type of pain can be experienced both in and out of shoes.
TREATMENT AND PREVENTION
Just because you have this deformity does not necessarily mean you have to have treatment. In the asymptomatic or non-painful deformity it is more prudent to find the underlying cause of the deformity and make changes accordingly.
Having said that, I can tell you that over the years I have had patients come to me with what appears like a golf ball growing on the inside of their foot and they swear to me that it does not hurt. If that is the case, leave it alone.
NON SURGICAL BUNION TREATMENT
Orthotics-So what an orthotic does in these cases is to reduce the over flattening of the foot which then results in an improved alignment of the joint and reduction of pain in the joint itself. The degree of relief is probably inversely proportional to the degree of damage that is already done. This means orthotics generally will work on mild to moderate bunion pain but not severe pain.
Keep in mind that orthotics especially in women will require a wider if not slightly longer shoe. So if a shoe that is tight and irritating a bunion to begin with has an orthotic added to it, the shoe becomes even tighter (and more painful).
This therapy will not make the existing deformity disappear, but it should slow down or eliminate further worsening of the condition. Follow this link for more information, hallux valgus and orthotics.
Sensible shoes-Elimination of shoes that are either too narrow, to flimsy in support, or too high in the heel. Trying to wear a narrow high style shoe with a large great toe deformity is like trying to put a square peg into a round hole; it just does not fit. This kind of mentality will eventually lead to a worsening of the condition.
do bunion splints work?
Cushions, braces and splints-that are sold for this condition are not my first choice because in most cases they just take up more space in the shoe and put more pressure on the bump. My only exception to this is in people who are experiencing "joint pain". The best bunion splint therefore, is one worn at night that will keep the toe straight but not create excessive pressure within the shoe.
I have also been known to use these splints after surgery, for a short time, in an effort to keep the joint properly aligned during the healing process. The splint on the left is for night use only, while the splint on the right is for day time use. Keep in mind, you can only wear laced casual shoes.
AGGRESSIVE TREATMENTS
Anti-inflammatory medication-is fine for short term use but should never be considered as a solution in that over the long haul the medication will lead to systemic problems in most individuals.
Cortisone injections-can be very helpful in those have bursitis pain and to a lesser extent for those suffering from joint pain.
Physical therapy-can be helpful in relieving flare ups.
CAN I FIX A BUNION WITHOUT SURGERY?
The question frequently asked of me is when to have surgery to correct this deformity. (It is estimated that over 200,000 people per year have hallux valgus surgery in the United States) My criteria is simple; when the pain of the deformity starts to affect your everyday life on a regular basis. You no longer golf, or go for daily walks, or go shopping with your friends out of fear that “my foot will start hurting”. Now the quality of your life is being affected. See my essay on surgical consideration.
Having said that, keep in mind that hallux valgus surgery is not without risks (as is any kind of surgery) and that the type of surgery your friend may have had, may not be the type you will require. The well trained podiatrist probably does at least a half dozen different types of procedures based primarily on the size of deformity. The type of procedure will usually determine the length of recuperation. The risks of hallux valgus surgery include the following:
- infection- (true in all types of surgery).
- loss of motion- (joint stiffness); the big toe does not bend, although in some procedures this is expected and the joint will no longer hurt.
- delayed healing- because of the dependent nature of the foot there is usually more swelling than in other parts of the body so healing may take longer.
- surgical failure- whereby you are no better off after surgery than you were before the procedure.
- nonunion- in procedures where the metatarsal bone has to be broken and re-set in an effort to re-angulate the bone, there is always the possibility that the broken bone will not heal.
- implant failure- in the case of a joint implant there is always the possibility it may have to be removed due to infection or reaction to the materials of the implant.
- recurrence of the deformity.

|
Think complications can't happen? This is a picture of an over-corrected bunion deformity; what is known as hallux varus. In an effort to move the big toe away from the second toe, the surgeon (someone else), moved the big toe too far in the opposite direction. Now the patient has even more trouble finding comfortable shoes and needless to say is quite unhappy with the appearance of her foot.
Even worse, the hallux varus throws off the "architecture" of the foot. Because the big toe and to a lesser extent, the second toe are in a "varus" position she has developed a painful corn on the end of her third toe.
The type of anesthesia used in this type of surgery ranges anywhere from local anesthesia where just the foot is put to sleep, to intravenous sedation (twilight sedation) with local anesthesia, to general anesthesia. The vast majority of my patients are done under local anesthesia with intravenous sedation on an outpatient basis.
I prefer this type of anesthesia because the patient feels no pain, is not having general anesthesia and all the potential risks associated with general anesthesia, and tends to be awake shortly after surgery with less chance of being "sick" from the anesthesia during the following 24 hours.
Hallux valgus surgery has become very sophisticated surgery; it is not just a question of removing the bump. Most of the procedures done attempt to realign the joint.(joint pain vs. bump pain) Discuss your surgical options with your doctor
CRITERIA FOR CHOOSING THE PROPER BUNION PROCEDURE
Some of the more common bunion procedures that are performed:
| Procedure Name | Type of Deformity | Procedure Highlights |
|---|---|---|
| Simple Bunionectomy | Mild | Only the bony protrusion (bump) is removed. Typically performed when the intermetatarsal angle is normal. |
| Austin Bunionectomy | Moderate | A common osteotomy where the bone is surgically broken at the neck, shifted for alignment, and fixated with hardware. |
| Lapiplasty | Moderate to Severe | Corrects the deformity at the metatarsal cuneiform joint to provide a stable, three-dimensional correction. |
| TightRope Fixation | Moderate | A "non-osteotomy" option using a high-tension wire and anchors to pull the metatarsals together without breaking the bone. |
| Joint Implant | Severe / Arthritic | Used when cartilage is eroded. The natural joint is replaced with an artificial one to restore motion. |
| Minimally Invasive Surgery | Mild (Bump only) | Uses a high-powered burr through a tiny incision to shave the bone, though it may risk ligament damage. |
Once the decision is made to have a bunion surgically corrected it now falls upon the surgeon to determine the type of procedure to be performed. Not all deformities are the same; that is essentially why one's surgical experience will probably differ from the next person.
When determining the type of procedure to be performed it is important to determine if the patient is having just bump pain, or just joint pain, or both as that will come into play in the decision process as to the type of procedure to be performed. Next, the surgeon will look at the various angles that are formed between the bones of the foot on x-ray. The accepted practice is to measure these bone angles which will help determine the type of procedure to be performed. There are easily a few dozen different procedures (and their variations) out there to repair bunions.
The decision as to which one to choose many times is based on the angles that are measured on the x-ray. (I cannot emphatically state that all doctors take the time to actually draw out these angles because there is a margin of error based on the position of the foot when the x-ray was taken and the actual accuracy of bisecting the bones in order to draw out the bunion angles).
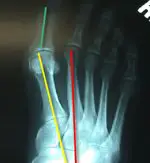
|
Look at the x-ray of a bunion to the right. These are two of the most common angles drawn out to evaluate which procedure to perform. (there are additional angles that may be taken into account based on the architecture of the foot in question). The angle formed between the yellow and red line is known as the intermetatarsal angle.
Normal is considered 8-10 degrees for this angle. As bunions progress, this angle actually widens. The first metatarsal bone actually moves away from the second metatarsal bone. Depending on how wide the angle is at the time of surgery various procedures are available to reduce this angle. If you do not reduce this angle sufficiently, there may still be problems with the bunion after just the "bump" is removed.
In general, the wider the angle, the greater the amount of work that has to be done to reduce the angle.

|
The video just below is that of an Austin bunionectomy, which is used to reduce a moderate intermetatarsal angle. This procedure is done at the level of the neck of the metatarsal. Larger angles may be reduced by doing procedures further back on the first metatarsal or even the joint just behind the first metatarsal bone. In general, one will be able to ambulate after a simple bunionectomy (just having the bump removed with a normal intermetatarsal angle, or even with a procedure done at the neck of the metatarsal such as the Austin, but procedures done further back will usually require a time period of being non-weightbearing.
The angle formed between the yellow and green line represents the hallux abductus angle or the deviation of the big toe (hallux) relative to the first metatarsal bones. If this angle is too large there are osteotomy procedures available (surgically breaking and re-aligning bone) to fix this angle as well.
Not only are the angles that form the bunion important, but the actual condition of the joint itself is also very important. If the cartilage making up the joint is too far eroded then even a procedure that creates perfect alignment of the joint is still going to be problematic for the patient.
It is at this point that the surgeon has to decide to either remodel the joint or replace the joint with an implant or artificial joint. Unfortunately, the only real way to know the actual condition of the joint is to visually inspect it, once the foot is open. In general older individuals who also happen to be more sedentary are better candidates for great toe joint implants because quite frankly there is a life expectancy to implants meaning they can and do wear out over time.
Here is a video of an Austin bunion surgery. The metatarsal bone is surgically broken with precise cuts in an effort to realign the bone (osteotomy). With the great fixation procedures that we have today people can walk after this bunion osteotomy.
As a side note new advances in medicine seem to be occurring on a daily basis. Bunion surgery is no different. The video you just viewed of an Austin bunionectomy shows one of the procedures we do to surgically break and reset bone (osteotomy) in an effort to move the first metatarsal bone closer to the second metatarsal bone to get better alignment of the big toe joint.
A new device called the TightRope fixation manufactured by Arthrex is a high tension wire that is placed through the first and second metatarsal bones in an effort to reduce the distance between the two bones. The beauty of this concept is that an osteotomy does not have to be performed. Since most bunion complications generally center around the osteotomy itself, having another option to reduce the intermetatarsal angle is very exciting.
If you look at the two x-rays below the one on the left is the preoperative x-ray. The goal of surgery as represented by the horizontal arrow is to move the first metatarsal bone closer to the second metatarsal. The x-ray on the right is the postoperative view and you can see the "tightrope" that has been drilled through both the first and second metatarsal bones and is held together by the black anchors.
I must caution you that the use of the TightRope for bunion correction is a relatively new concept but is very promising.
Update November 2010 After having read a recent study regarding the TightRope procedure I thought I would pass along some of the findings. Please keep in mind this was a very small study and it was done on people who had the procedure performed two years ago or less. (This procedure, like most medical procedures need to be examined at least five years down the road with a large patient population.)
The most common complication from this type of procedure has been fracturing of the second metatarsal bone which in all cases required further surgery to correct the fracture. There are a number of reasons this may happen. If the bone stock is not adequate, meaning there is a reasonable amount of osteoporosis or osteopenia, whereby the overall calcification is diminished. Of course this is a problem that should be looked at pre-operatively in any potential candidate.
Secondly, one also needs to evaluate the overall thickness of the second metatarsal bone. Many people exhibit a very thin second metatarsal bone relative to the first metatarsal and to expect the thinner bone to support the larger bone may be a bit of a stretch. This too should be evaluated pre-operatively.
The study mentions other possible causes for failure such as the fact that the drill holes through the second metatarsal bone will naturally weaken the bone. In addition they mention the fact that the first metatarsal bone has its own range of motion independent from the other metatarsal bones, thus putting more stress on the second metatarsal bone.
Exacerbating the problem is the fact that the tension wire itself is made of a hard abrasive suturing material that over time in connection with the movement of the first metatarsal will cause a "sawing" motion on the second metatarsal and will eventually weaken the bone.
If any of you reading this section are contemplating having this procedure done, please discuss these potential complications with your surgeon.

|
|
Update June 2016 In an effort to refine the tightRope procedure, other companies have come out with different variations of the hardware used for this type of correction. One company, Arthrosurface, has come out with a device known as the KISSloc Suspensory Suture System.
|
The next video demonstrates implant surgery for correction of a bunion.
As just mentioned, this is generally done when your doctor determines that the cartilage is too worn out to be salvaged and is then replaced by an artificial joint. This procedure is sometimes performed in conjunction with an osteotomy procedure to realign the metatarsal and toe bones.
Many patients ask me if you can have laser surgery on bunions. The answer is no. Theoretically you could use a co2 laser to make the skin incision (which I have done) but it really affords no advantage over a regular scalpel incision. More importantly, lasers cannot remove bone, all they do is burn bone, so a laser could not be used to remove the large bump of a bunion deformity.
minimally invasive bunion surgery
For those individuals that have a painful bump on the inside of the foot and the angle between the first and second metatarsals is essentially normal, many times just the "bump" can be removed through a very small incision. Using a high powered burr, the enlarged bone can be burred away resulting in an elimination of the bony protrusion. The problem I have always had with this procedure is that in the process of burring away excess bone, the surrounding soft tissue structures, primarily the capsular and collateral ligaments will also be destroyed. Destruction to these ligaments may adversely affect the function of the big toe joint in the future.
RECOVERY FROM BUNION SURGERY
what to expect after bunion surgery
Recovery time after bunion surgery will vary depending on a number of factors.
Probably the most important factor is the type of bunion surgery performed. People will generally recover quicker with a more simpler procedure. The more complicated procedures take longer to heal, then there is also the time period afterwards to rehabilitate the joint generally through physical therapy.
This does not mean you are not walking after bunion surgery; in most cases the patient is walking immediately. By this I mean you can ambulate from day one (there are some bunion procedures where you have to be nonweightbearing for a period of time; discuss this with your doctor), meaning you will be able to get around and take care of yourself but by no means will you be on the golf course.
In an otherwise healthy individual who has undergone an osteotomy (surgical breaking and re-alignment) for their bunion deformity, in most cases it will take 6-8 weeks for the surgical site to completely heal. Virtually all osteotomies are fixated with hardware such as screws, plates, k-wires, wire suture, etc. to keep the alignment in position. So even if your surgeon allows you to bear weight and walk on your foot it will be with limitations until the fracture has completely healed.
In simpler bunion procedures where there are no bones surgically broken and in cases of implants for the great toe joint, the current thinking is to get the patient walking as soon as possible in an effort to exercise the joint and reduce the possibility of joint stiffness which in itself can become an issue.
Other factors that will affect the recovery time after bunion surgery include your age, younger people tend to heal quicker, your overall health, and maybe the most important factor is patient compliance. Follow your doctor's postoperative orders for home care and mobilization. Generally, when patients are noncompliant they will run into more postoperative problems.
Time of year-As previously mentioned, because of the dependent nature of feet, they tend to swell in hot weather. The older you are, the more they swell. Foot surgery also causes feet to swell simply because the body's way of healing an injured area is to increase the blood flow to the area bringing with it nutrients that facilitate healing.
So, if you have foot surgery in hot weather, the combination of the surgery and heat may keep your foot swollen for a longer period to time then if you had your surgery in cooler weather. The time of year should not be your sole criteria for when to have surgery, but it certainly should be part of the decision making process.
exercise after bunion surgery
The two general questions I am usually asked by patients is "when can I return to sports?" and in the case of women, "when can I start wearing heels?". There is no clear cut answer to these questions since every one heals at a different rate. If your surgeon is an experienced surgeon, he or she will be able to give you guidance in answer to your questions.
The goal in this day and age is to get our patients walking as soon as possible in an effort to keep the newly remodeled joint moving. Years ago the thinking was to keep the patient in bed so that the joint could heal; the problem with that line of logic was that the joint tended to get stiff and it would take even longer to rehabilitate. So, essentially, you will be exercising the bunion joint fairly quickly after surgery, but as far as returning to exercising, that decision should be left to your surgeon.
There is some controversy in the medical community about the benefit of physical therapy after surgery. I do not send all my patients for physical therapy; in fact in many cases I will just give them instructions in exercises and other things they can do at home to facilitate their healing (and only hope they actually follow my instructions).
Most experienced surgeons can get a "feel" for when a patient is not progressing along a normal healing time line. In those instances and in situations where a patient may develop a problem, physical therapy by a physical therapist becomes more important.
Once your sutures have been removed and if not in a cast, you will be ready for a shoe. This does not mean your everyday shoes. Some doctors like to have their patients wear a daytime bunion splint to maintain their surgical correction. This plus the fact that your foot will be swollen (a normal part of healing) will make it impossible to wear the shoes you already own.
I generally have my patients buy an inexpensive pair of sneakers large enough to accommodate the enlarged foot and splint; this seems to work out well. If you were given a surgical shoe to wear you want to get out of that for two reasons. One, it limits motion in the joint, which we do not want and secondly patients start complaining of back pain, plus, you cannot drive with a surgical shoe if it is on your right foot.
One of the newest bunion procedures being performed today is the Lapiplasty procedure. It is a novel approach to an older technique where the correction of the bunion is made at the level of the metatarsal cuneiform joint. It is done in such a manner to a yield a more stable correction, thus increasing the chance of a positive outcome. See the videos below:
Para traducir esta pagina, ve al boton de traduccion de Google en las esquina superior derecha de la pagina
TAILORS BUNION
While we are on the subject of bunions we should also discuss the condition known as tailors bunion. This is a bunion deformity on the outside of the foot, sometime referred to as a fifth metatarsal bunion.
In the picture below you will notice the location of a tailors bunion.
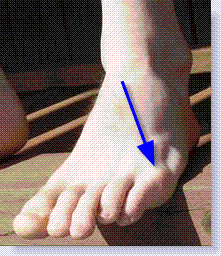
|
This condition got its name from the turn of the last century when tailors would spend long hours working with their feet crossed in such a manner that the outside of the feet would continually press against the floor and as a result, over time, the bump on the outside of the foot would form.
This condition can be an acquired problem such as the example above or a congenital problem where there is a flare laterally of the fifth metatarsal bone resulting in the head of the bone being very prominent.
In either case the foot now has trouble fitting into a conventional shoe, (it is too wide). If there is enough pressure on the bone a secondary bursitis may form which will make the pain even worse. In those with poor circulation the skin overlying the bone may breakdown from too much pressure.
A tailors bunion will generally only hurt in shoes and be fine barefoot, or in open shoes like a sandal.
So now that we know the major precipitating factor is shoes, the sensible move would be to avoid shoes that aggravate the condition. Shoes that are too narrow, or have too high a heel, or are made of very stiff material will all go a long way to aggravating the tailors bunion.
You can always try padding over the tailors bunion but I generally find that to be a waste of time. All the pad does is take up more room and cause the tailors bunion to hurt more.If there is an inflamed bursal sac, a cortisone injection can be very helpful with the understanding that if you do not modify your shoe selection, the problem will eventually return.
Anti-inflammatory medication can be tried but I find it is rarely helpful by itself.
If all else fails there is always surgical intervention. A tailors bunion is different than the classic bunion in that in this type of bunion we do not really have to worry about biomechanical considerations.
Sometimes going in and removing the enlarged bone is all that is necessary, but in general, if there is a real lateral flare to the fifth metatarsal bone, an osteotomy (cutting and resetting of the bone to change its angulation) may be necessary.
Frequently Asked Questions About Bunions
1. Can I fix a bunion without surgery?
While non-surgical treatments like custom orthotics, splints, and wide-toed shoes can significantly reduce pain and slow the progression of the deformity, they cannot physically "remove" the bony bump. Surgery is the only way to anatomically realign the joint.
2. Are bunions caused by wearing high heels?
High heels and tight shoes aggravate the condition, but they are rarely the primary cause. Most bunions are the result of inherited foot structure and poor biomechanics (such as excessive pronation) that place undue stress on the big toe joint over time.
3. How long is the recovery time after bunion surgery?
Recovery depends on the complexity of the procedure. For a standard osteotomy (cutting and resetting bone), it typically takes 6-8 weeks for the bone to heal. However, many modern procedures allow for weight-bearing and walking much sooner than older techniques.
4. What is the difference between a bunion and a Tailor's bunion?
A standard bunion (hallux valgus) occurs at the base of the big toe on the inside of the foot. A Tailor's bunion (bunionette) occurs at the base of the fifth metatarsal (little toe) on the outside of the foot.
5. When is the right time to consider surgical correction?
Dr. Mitnick recommends surgery when the pain begins to interfere with your quality of life—preventing you from exercising, shopping, or performing daily activities comfortably. If the deformity is asymptomatic (not painful), it is often better to manage it with orthotics rather than surgery.
REFERENCES
Questions I have Answered From Visitors
Bunion returned 3 months after chevron osteotomy
I had/have bunions on both feet. The right was much more severe than the left...my big toe was starting to cross under my 2nd toe. I had a chevron osteotomy with distal soft tissue procedure in September. There was a pin between the big toe and the 2nd toe holding the bones in place during healing and I was in a darco boot that kept me from putting pressure on the forefoot.
After I was recovered, my foot looked great other than some bruising and slight swelling. My toe was nice and straight. It was a little stiff, but nothing too bad. 3 months later my toe has started to drift back over and the protrusion seems to have gotten bigger and my toe pops more now. Whenever I move my big toe out to stretch it, the joint pops.
After I was allowed to wear shoes again I got a pair of very wide, flat comfy plush lined boots that felt like house shoes and put no pressure on my healing foot. I have worn those everyday since. Did I do something wrong, did the surgeon not do a good job or am I just cursed to have old lady feet in my 30's? I know bunion surgery sometimes has to be repeated, but only 3 months later? I thought years.
Response:
Hi Amanda, You are right, bunions should not return after three months, particularly procedures where an osteotomy (surgical breaking and re-aligning of bone) has been performed. If you followed your surgeon's advice from day one until the time he told you to go about your business and resume your life, then whatever problems you are having are probably not your fault.
If I could see an x-ray, I probably could be more helpful in advising you, as the x-ray will tell a better "story" of what is going on here. You mention that the big toe is moving back towards the second toe. I have to say, in most bunion procedures the big toe does drift somewhat closer to the second toe over time, but if your big toe is back under the second toe, or approaching that position, then there is a problem.
I would also be curious to know if there is any pain associated with your corrected foot, besides the popping. One could make the argument that if you are not having pain and the big toe has only drifted a small amount and is not back under the second toe, then the procedure should be considered a success. If, however, the big toe has moved back a great deal and there is pain, then there is a problem.
Because of the amount of time that passed before the toe started to drift back, I would guess there is no problem with the actual osteotomy. If the osteotomy failed you would probably be having a lot of pain. Instead of me sitting here trying to guess what is going on, my best suggestion would be to get a second opinion from a surgeon in your area. You need someone involved who can give an unbiased opinion of what is going on, as many times you will not get an honest opinion from your original surgeon.
If it ends up that the osteotomy is fine and there is minimal to no pain, then I would suggest you live with what you have. You may require surgery years down the road simply because you are so young, but the one thing you do not want to get involved with is surgery after surgery. Multiple surgeries in the same area have a higher propensity for failure due to the normal scarring that occurs after each procedure.
Foot-Pain-Explained.com
Question from: Ann
Location: Charlotte, NC
Patient Question:
"I recently posted a question about pain after bunion surgery and wanted to follow up with the 2nd opinion... I had a right bunionectomy in March 2017. I started having pain on the bottom of my foot at the 2nd and 3rd metatarsal heads approximately 5-6 months post op. I also experience pain in my entire 2nd toe, especially if I bend it towards the floor... Can a doctor actually 'over correct' when doing a bunionectomy and this cause pain? Do those with metatarsalgia experience pain in the 2nd toe?"
Dr. Mitnick's Response:
Hi Ann,
There is such a thing as over-correction of bunions, but that is where the big toe ends up in the complete opposite direction, which is not your case.
Because you had a Chevron osteotomy on the first metatarsal, the surgeon may have shortened the first metatarsal. This happens with this type of cut, and if the bone was already short to begin with, a weight-bearing imbalance is common. This is why your surgeon wants to cut the second and third metatarsals—to try and create a better alignment.
Recommended Next Steps:
- Imaging: I suggest an MRI (or ultrasound if insurance won't cover it) of the second and third metatarsophalangeal joints to see if the ligaments attaching the metatarsal bones to the base of the toes are torn.
- Conservative Care: If the ligaments are torn and you want to avoid further surgery, you would need to use a walking boot for a period of time.
- Orthotic Adjustment: If the ligaments are not torn, you need a custom orthotic with a metatarsal pad built in to lift the metatarsal heads. Your doctor can experiment with softer or flatter pads if the current elevation is uncomfortable.
Marc Mitnick, DPM
Visitor Name: Beverly
Location: Alabama
I have changed my shoes from all leather to a running shoe that has mesh in the top of the foot area. They are also a straighter shoe (meaning a little wider at the toes) and that has helped quite a bit. He also told me to use Oragel for pain, soak in Epsom Saltz and use my Pedegg or a pumice stone to keep it smoothed down.
It's only been a week now, but I'm still hurting about as much as before. I keep telling myself it will be better once it heals.
Hi Beverly,
Its not what I would do, but that does not make it wrong. My issue is with the fact that the "seed corn" very well may come back.
The callus and small cyst is from too much pressure from the shoe on the underlying bone; the skin then gets caught in between and the callus and and cyst form. The problem here is that you have done nothing to change all that, so you can assume the problem will return.
What you need to do is identify the shoes that aggravate this problem, avoid wearing them. Even still the growth may come back but possibly not as frequent. If and when it does come back, ask your doctor to not be so dramatic and just trimm the callus and carve out (curette) the small cyst. The "hole" you are left with should be just slightly larger than the small cyst. You will get immediate relief and will not have to do anything at home for it afterwards.
Marc B. Mitnick, DPM
Visitor Name: Arthur
Location: Massachusetts
I have bunions on both feet, though they cause infrequent pain or trouble. However, on my left foot, I also have a tailor's bunion that flared up about four months ago and was diagnosed about two months ago. The angle is quite large and the doctor recommended an osteotomy.
There is pain on the side, at the leftmost point of the bunionette, but the greatest pain is actually on the bottom of the bunionette. It is almost impossible to walk on a hard floor barefoot. And even in padded, wide shoes, there is pain on the bottom of the foot, below the bunionette. I frequently tape a pad in the middle of the forefoot to narrow the foot a little and put less pressure on the area below the fifth metatarsal. All this has affected my gait and led to pain in other parts of the foot and ankle. By the way, I am naturally slew footed, though the skew on the left side is more pronounced.
I am an active hiker and distance runner, 56, average-to-light weight. Are there realistic options for repairing this short of the osteotomy, the main downside of which is six weeks of immobility and major loss of muscle? I've seen that in some cases resection may be an option, with far less downtime, and just noticed a tightrope procedure that is promising but doesn't have much history. What are the stats on recovery? What percentge of active people who undergo the osteotomy return to the same level of activity?
Many thanks for your advice,
Art
Hi Art,
If the lion's share of pain is on the bottom of the foot then any surgery anticipated has to have as its goal, elevation of the metatarsal bone and not necessarily decreasing the space between the fourth and fifth metatarsal heads.
Most cases of pain underneath are due to either a severely prominent fifth metatarsal head thus putting more pressure on the walking surface, or, a lack of plantar fat underneath the metatarsal head thus causing a lack of cushioning for the metatarsal, or, an inflamed bursitis underneath the metatarsal head.
The order in which I treat this would be:
- Accomodative padding in an effort to take pressure off the metatarsal head.
- If there is an inflamed bursitis, I would consider a cortisone injection.
- Instead of an osteotomy, I might consider just a condylectomy which is a shaving away of the bottom of the metatarsal head in an effort to decrease the pressure exerted by the bone on the walking surface.
A condylectomy is a much simpler procedure than an osteotomy, with a quicker healing time, and no threat of non-union of the osteotomy, since an osteotomy is not being performed.
The tightrope procedure as I know it is reserved for bunion corrections and not tailor bunions.
Marc B. Mitnick, DPM
Foot is deformed 1 year after surgery
Visitor's question
I had bunion and hammertoe surgery about a year ago on my left foot. Instead of removing the bunion the doctor just shaved it. As a result, when it healed, my big toe healed severely bent to the left. It pushed the toe next to it out of joint and now it is crossed over the middle toe and won't straighten out.
I have to wear a foam piece to keep my toes from rubbing together. I used to be able to wear “B” width shoes but now my left foot is one and one‑quarter inches wider than my right foot. The bunion is bigger than it was before the surgery. Even extra‑wide shoes don't fit on my left foot without hurting.
I went to my doctor and he said to live with it — my foot will always be wider. I have a lot of skin breakdown on the second toe because since it crosses over the middle toe, it rubs against all my shoes. My foot was relatively normal before the surgery but now it looks deformed, kind of like a clenched fist.
Would a surgeon be able to straighten out my toes and rework the bunion? It hurts all the time so I am mainly concerned about pain relief and being able to wear normal shoes again. I included a picture of both feet for comparison.
Doctor's answer
Hi Anna,
Unfortunately, there are no pictures included with your post. Speaking in general terms, your foot may require additional surgery. Yes, having included pictures might have been helpful to offer a more specific opinion, but I will try to answer your question regardless.
When we as foot surgeons evaluate bunions, we do so from a structural standpoint — reviewing X‑rays and measuring the angles formed between the first and second metatarsal bones, as well as the angle formed between the first metatarsal bone and the big toe.
We also look at the quality of the big toe joint as it appears on X‑ray, although in most cases the quality of the joint is usually worse on actual inspection during surgery.
We also evaluate bunions based on the needs of the patient. What I mean by that is: just because an X‑ray may suggest one type of procedure, the needs of the patient may suggest that they can get by with a different procedure — usually one that requires less work and therefore a quicker recovery time.
Sometimes a lesser procedure has to be performed simply because the patient is not a good candidate for a more involved procedure. I do not know how old you are, but older individuals who may exhibit osteoporosis or who are chronic smokers may not heal well from more complex procedures.
That said, in cases where a lesser procedure is done — such as simply shaving the metatarsal bone — the result should still be some degree of improvement, not a worsening of the condition.
I have no way of knowing why your big toe moved further away after your surgery. The most obvious reason, though not the only one, would be that the surgeon did a poor job of closing the joint after the “bump” was removed.
Assuming you are reasonably young and in good health, you could consider additional surgery to re‑straighten the big toe joint, as well as possible surgery on the second or even third toe to better align the toes. More than likely, this will be a much more involved procedure and will require more sacrifice on your part.
If pain is your primary motivation, then by all means seek an opinion from another surgeon — and perhaps even a third — to determine the best course of action. The problem with “re‑dos” is that they present special challenges, so having more than one opinion can be very helpful in deciding whether further surgery is right for you.
Marc Mitnick DPM
If you happen to live in the New York - New Jersey area and would like to visit our office
|
|
To make an appointment online or for directions to our office click Dr. Marc Mitnick.
DISCLAIMER: The purpose of this site is purely informational in nature. It is not intended to diagnose, treat or cure any medical condition. This information is not a substitute for advice from a medical professional. Please consult your healthcare provider for accurate diagnosis and treatment. The information presented here may be subject to errors and omissions.
SITE LAST UPDATED: MAY 2026


I've been doing some aggressive research lately (it's how I found your incredible website) and realize now that my symptoms are not consistant with the diagnosis.
Jennifer
Hunterville, NC
….after reviewing your amazing site (great for the avg. jill). So thank you very much!!!
Liesbeth
NY
I am really, really impressed with your plain-speak explanations for the various conditions.
Jacqueline
NJ
This was an extremely helpful site. I have an appointment on the 18th and your info. Was right on target…..
Jack
Fla
A well organized site containing much information written in a manner that the average reader can comprehend.
Jean
Ontario, Canada
I found your website and articles most interesting.
Andrew
Fla.
Thank you for a quick response. I think your site is the best information site on foot pain and I have viewed many.
Judy
(location unknown)
I came to your website, footspecialist.net via www.foot-pain explained .com which I think is also your website? I thought explanations for different types of problems were well addressed and thoughtfully stated for the patient in mind.
L.W.
New York
You have an amazing and extremely informative site. I enjoyed looking through all of the data and stats.
Yvette
Memphis, TN
Thanks again so much for the information in the article. Very interesting.
Anna
Scotland
Great article. I have had plantar fasciitis since I was in high school……..
J. Simmons
(location unknown)
Dear Dr. Mitnick, The orthotics arrived four days ago and I slipped them into my shoes immediately. I was skeptical as to the usefulness of the item, they really didn't look very exotic. I have to say though, after using them for just four days, I have experienced grand relief from my foot pain. Even the very first day, I was able to do a lot of work while on my feet with at least a 75% reduction of pain. It has only gotten better every day, and I go nowhere without my shoes with the orthotics. I had been experiencing extreme heel and sole pain for about six months and had to take extended breaks off my feet many times a day as well as regular doses of Ibuprofen. Since getting the orthotics, my life has returned to normal and I feel good again. Just wanted to say thanks for the recommendation for a very effective item, I had no idea what a change this item could affect.
Yours truly,
J.C. Forbes
Tennessee
Thanks for the Response, you hit it on the head.
Steve
Redondo Beach, CA
Thank you for your time and expertise in answering my question…..
LH
(location unknown)
First, thanks for putting together this website. Its the most informative site I have found dealing with foot problems. Last June I started having pain and swelling at …….
Joe
(location unknown)
First of all, thank you for having all this useful information available in one place. I've been through most of your website and based on my research, pain and evaluations I think I've narrowed things down quite a bit.
Pete M.
(location unknown)
Thank you for the best site I have found when researching foot pain.
Glenda B.
Madison, Alabama
Thanks for replying so quickly. I was a bit concerned. I think your website is great, and chock full of info.....
Carol
Denison, TX
Dr. Marc, Thank you so much for your reply which seemed to be right on. I have researched many sites but you put me on the right path to the possible answer. My foot pain may not rule the rest of my life after all! I believe I'll make a sign that reads, "THE END IS NEAR!" Thanks Very Much,
Dawn
West lafayette, IN
Dear sir...no doubt you get positive comments re your site...May I please be added to the list of your admirers. In all of my years of web surfing I would say your site is right there with the very best. Thank you for taking the time to write the terrific info you provide and for putting things into laymen terms for us mere mortals. I pray you have much on going success and thank you again for a deed well done. As for me I did not find much help for my symptoms and will continue on my quest. Were you anywhere in the South I would make and appointment...Thanks again dear sir...m.e.
Michael E.
Tampa, Florida 33624
Hi. This is a great site! I'm a healthy middle aged woman who is in good health, but.....
Kelly
Texas
Just a wee word of thanks for your wonderful website...It is a terrific service...Thank you for providing your knowledge and help...With highest regards, m ebeling
Michael D. Ebeling
Tampa, Florida 33624
Thanks for a most interesting website, which has helped a lot.
Steve
UK
Dear Dr.Mitnick
I usually do my research on the Mayo clinic website. I think your website is the most informative site I have found when researching foot pain.
I thank you for putting together this incredible website.
Regards,
Dragica W.
Edmonton,Canada
....I have been told that it is not hard enough to be cut off. Please help, I am not sure what to do now! THANKS FOR A WONDERFUL AND VERY HELPFUL SITE!
Roxy
South Africa
You have an unusually clear, informative and well-written website for laypersons. Thank you for that.
Matthew W.
Mansfield Ctr, CT
First, I'd like to thank you for all the information that you provide on your website and the opportunity to write to you.
Steve
Placentia, California
First, I want to let you know that you have the best web site I've found related to foot issues. (The only thing I had difficulty finding was the "ask a question" page.)
Unknown
Unknown location
I received the orthotics Monday afternoon and began wearing them Tuesday. After two days I would say that I have noticed a huge improvement in the discomfort I have been experiencing. My foot feels better than it has in months.
Ric J.
Unknown location
I greatly admire someone like you who would donate and dedicate so much time and effort to helping strangers with no compensation. Truly, it is uncommonly kind. And your site is so intelligently arranged.
Ron R.
Pacific Grove, CA
I used to work for a podiatrist (front desk) back during summers in college years ago, so I know the benefits of good care. Again, I want to thank you for an EXCELLENT website. It was so great to get to your site (top of google search) and actually find all the answers I needed EASILY and QUICKLY! Clearly you put a ton of work into it and I really appreciate it.
All the best,
Victoria
Alameda, California
By the way, millions of websites could use yours as a guideline on how to organize information and make the site user-friendly. Kudos to you!
Anonymous
Thank you for your very interesting and informative site!
Anonymous
Hi. I come to your site often looking for information. It is really informative and I appreciate it very much. I have RA and have been having considerable amount of foot pain...... Dee RN
Thanks very much for the wonderful informative site.
Catherine
New Zealand
Thank You for my answer! I have been schedule for a bone density scan, allingment, and I am in the process of getting orthotics made, and checking out the natural remedies. Thank again! What a great web site!
Sincerely
Josette
Yes I want both pair of orthotics. You don't have an option of ordering 2 at one time so I had to place the order twice. Thanks. My husband likes these and wants to put them in all of his shoes. (referring to Superstep orthotics)
Cindy H.
Arizona
I searched the internet everywhere for a clear description and illustration of my symptoms/problem. https://www.foot-pain-explained.com/ was where I ended my search with answers. If I lived in Jersey (left 30 years ago) and didn't live in Florida I would definetly make an appointment with Dr. Mitnick.
Thanks, Kathy
Florida
1st of all THANKS A LOT for your great site......
Anna
Poland
Thank you so much for your response. I will let you know how I am doing if you would like. Your website is awesome!
M P
South Carolina
Hello! I want to thank you for such an informative website! I found you based on my ankle pain search and am happy to realize that there may be a relatively simple cause and solution....
Natalie
unknown location
...Thanks for your fantastic service.
Gary
Arlington, VA
Thank you so very much, that would be much appreciated. I love those insoles, by the way. (referring to Superstep orthotics)
Kelly W.
San Clemente, CA
Dr Marc is fantastic...He seems to know exactly what you are feeling with the problems you are having. I wish he was in my home town so I could go to him with my problems!!!!!!!!!!!!!
Pam
location unknown
Great insights! Thanks Doc, you're the best.
Glen
location unknown
I have been experiencing foot pain of various sorts and am working to figure out what it is. I found this site and can only say BRAVO!! What an excellent site! The time it must have taken to put all this together must've been a daunting task! I am sure it has helped so many people. Thank you so very much for doing this.
Bre
location unknown
Dr. Mitnick, Thank you so much for your reply. I did let my physician know and they took an x-ray - all is well! Also, thank you for providing this wonderful site, it is very helpful with lots of useful information! I appreciate your gift of time! God bless.
anonymous
Dr. Mitnick, Thank you, you were 100% correct. The pain finally brought me to the ER. I spent 8 days in the hospital. The Doppler you spoke of was able to show that there was no pulse in that foot. This was an arterial clot that split and traveled throughout my leg. My leg was almost amputated. I am in rough shape but have all my parts intact!! You certainly know what you are talking about. Thank you for taking the time to answer. Yours Truly!
anonymous
Staying at home after hallux surgery I spend quite a lot of time seaching info useful for avoiding problems which might come back. Today I found your site and I am .... delighted it happened. It's one of the best site I found last days.
Anna
Poland
Thanks for taking time to read and answer so many questions. It is truly a public service!
Esh
Seattle, WA
I just wanted to say that I am very greatful for this website!!
Bonnie
location unknown
Also, and importantly, just want to praise this web site. Thorough and thoughtfully presented, it certainly must be of considerable assistance to anyone with a foot problem. Terrific -- and very interesting.I trust the address comes up easily for those seeking information.
Bill
New Jersey
Thanks so much for answering my question. You've been more help to me than my own Dr. has been lately. Thanks again....I hope to be able to walk without pain someday.
Debbie
location unknown
Wow, that is exactly the information needed!!! thank you thank you thank you!!! I appreciate this help so very much from Marc Mitnick DPM. Excellent information and help to improve One's life.
Chrissy
location unknown
Thanks so much for this website Dr. Marc! It is so nice that you have this ask the doctor feature..I'm sure I'ts been helpful for alot of people. I will try what you suggested and see if it helps...thanks again!
Tracy
Evansville, IA
Dear Marc
I just want to say thank you for the quick response and the good info. I find it amazing and a super nice thing that you do here by answering medical questions at no charge.
Russ W.
location unknown
Your website is full of a lot of helpful information, and I am very impressed with the time in which you responded to my post. Thank you again for your time and consideration in your response.
-Sunny.
location unknown
Thank you very much for the information, I will consider it. Excellent web site.
Jackie
San Diego, CA
Dr. Mitnick, Just want to say thank you so very much for your quick response and very informative reply! After reading what you had to say, I called the doctor's office and was able to get in and see him the same day as my injury. Toe was x-rayed and luckily, it is not broken or fractured. Very badly bruised and will probably lose the toe nail. And although my toe and toe nail are still very black and blue and very sore, they ARE both starting to feel a little better. So again, thank you! I am so very happy that I came across your website. The service you provide is outstanding and immeasurable!
Rivi,
Albany, NY
Thank you so much for all of your advice. In searching the web for people dealing with this same issue i can tell you that you are a Knight In shining Armor! If I lived in Jersey I would gladly be your Spokesperson. Hopefully next time you hear from me it will be good news. God Bless,
Jill S.
location unknown
THANK YOU SO VERY MUCH FOR YOUR TIME AND EFFORTS, YOU ARE SO VERY APPRECIATED. THANK YOU FOR ALL YOU DO.
Jackie
Whichita, KS
thanks again, this site is very helpful.
mark
Boston, MA
Like others have stated...This site is amazing and I am so thankful that it was created.
....Keep up what your doing. Your a life saver.
Michelle
Colorado
Thanks again for the information provided on your site. It's easy for non-medical folk to understand your writing, and helps provide better communication between patient and doctor.
annielou
Colorado
Wonderful advice
by: Anonymous
This is the best site for foot problem info.
Thank you for this information. This description fits my pain and inflammation behind my 2nd toe perfectly.
by: Max
location unknown
Again, I really appreciate that you responded to my inquiry, and that your mention of Parkinson's helped me to find my way to a diagnosis of this difficult to diagnose disease. Most patients see on average 16 doctors before they are diagnosed. I hope that you can help other people that ask for your expertise in the future.
Barb D.
Canada
I just wanted to say that I am very greatful for this website!! I have had a fusion in my rt foot and am finally getting a little bit better......
Bonnie
location unknown
Again, Thank you from the bottom of my heart for taking the time to answer my question....your an angel!
Nancie
Wisconsin
Thank you for your response. You have provided some great insight (to my question)....
Julie
location unknown
Thank-you so very much for responding so quickly and in such detail to my question!! I will give my surgeon a call today!! This website is terrific!!!! Thank-you again!
Renae
North Carolina
Many Thanks Dr Marc!
Thank you for your response. It sounds like a good plan to me. He did not cut the wart out first ...
KG
location unknown
Thanks again doc for having this website and we STILL need qualified Podiatrists in beautiful sunny Tampa Bay (Bradenton) Florida.
Bessie Mae
Florida
Dear Dr. Mitnick, Thank you so very much for taking your time to answer my question. You have greatly relieved my anxiety related to the continual tingly I feel in my feet. I will share your response with my podiatrist next week. God bless you for having this question and answer page on your website! Most gratefully,
Lynne T.
location unknown
Your webpage is excellent, I commend you on sharing your knowledge to the public.
Robert
New Jersey
Thank you. you were more detailed than what others have told me they finally called from the last xrays and my son is now in a cast for 2 weeks he did have a fracture that was not noticeable.
a mom
location unknown
I have read your website and I have to admit that I am amazed at all the information that is on here. I have learned more than the three years I have been going to several doctors that I have seen!!
Melody
Lenoir, NC
Thank you so much Doc for a quick and thorough response!
Rustam
Bellevue, WA
I cannot thank you enough for your response, opinion, and suggestions! I want you to know how much it means to me, and I'm sure everyone else who has ever asked you a question! I feel like you're a lifesaver and have empowered me to take a stronger role and stand up for myself and my feet!
Jodi
location unknown
Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…