Not what you're looking for? CLICK HERE INSTEAD
The response to the question below was authored by Marc Mitnick DPM
foot aching
by Benjamin
(Loveland, CO)
At rest my left foot is fine. When I first stand up my foot aches in the area where my toes meet my foot. It seems to radiate across the top. Mostly as I am stepping forward with my right foot and my left foot is bearing my weight in the extended position. If I walk for a while, the pain seems to subside a little and become more bearable. But, as soon as I get off my feet for a bit and stand up, the ache is back full on. I went to a specialist and he didn't see anything in the x-rays, so he was really pushing these $500 shoe inserts on me. I don't feel like spending that kind of money on something if he can't even tell me what's wrong. I was thinking it could be a stress fracture or arthritis? I am 43 years old. Mildly active.
RESPONSE
Hi Benjamin,
I kind of agree with you; if the doctor cannot give you a diagnosis, how does he know that custom orthotics are going to help you?
In any event here are a few thoughts.
I do not think you have a stress fracture, even though your area of pain is a common site for this type of problem. For openers, stress fractures would tend to hurt more as you walk, while you state the pain seems to subside somewhat. Additionally, you state that the pain travels throughout the top of the foot, whereas a stress fracture of one bone would tend to hurt primarily in that particular area.
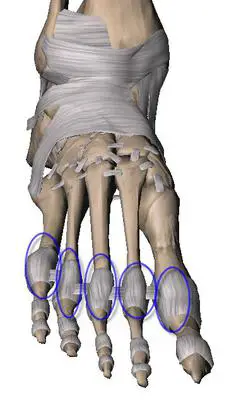
Moving further along, just because your x-ray does not look abnormal, this does not mean you do not have the beginnings of arthritis in what would be the metatarsal phalangeal joint, which is where your toes articulate with the rest of your foot.
At age 43 you are at the point where arthritis starts to invade every human being. The beginnings of arthritis could be nothing more than a narrowing of the metatarsal phalangeal joint which to some would still appear normal. Additionally, the cardinal sign of early arthritis is what is known as "morning stiffness" where the affected joints hurt when you first start to use them after they have been at rest. Generally the pain will then start to subside as you continue to use them. Sound
Depending on how much pain you experience when you first start to walk on your foot determines what needs to be done. Obviously, your foot hurt enough to seek out medical attention.
The first thing I would look at are the shoes that you wear. Shoes such as flip-flops, boat shoes and being barefoot a lot will cause excess bending at the metatarsal-phalangeal joint and this can inflame the joint. Wearing more rigid shoes such as sneakers or thick soled dress shoes limit the excess motion at the joint and this can help relieve your symptoms. So that would be the first change I would recommend.
Secondly, if you can tolerate them, I would start on a round of anti-inflammatory medication such as Aleve, Motrin, or Advil and take the medication on a daily basis , say for ten days, as directed on the packaging. That may go a long way to "quiet" down the inflammation.
You could try an orthotic to stabilize the foot and reduce the excess bending of the toes. At this point you should try a medical grade over the counter orthotic such as the ones we sell on this site; to see if the concept of an orthotic is helpful. A custom made orthotic might be something to consider down the road, but it should not be your first line of defense.
You may find that by trying some or all of these suggestions, you are able to quiet down the problem as it is very common for this type of pain to resolve itself.
Having said all that, I would be remiss if I did not mention the possibility of extensor tendonitis as the cause of your pain. This is an inflammation of the tendons that bring your toes upward. Again, from excess motion in the foot, these tendons can become inflamed and hurt in the area where you are experiencing pain. But, like a stress fracture, this pain would tend to worsen the more you walk, while you state your pain tends to lessen. The treatment for this, at least the "try it on your own treatment" would be the same as already described.
If you cannot resolve the pain on your own, you may want to consider a cortisone injection into the area or perhaps some physical therapy.
Marc Mitnick DPM
DISCLAIMER
ADDITIONAL REFERENCES
University of Rochester Medical Center
American Academy of Pediatrics
Columbia University Department of Rehabilitation
Illinois Bone and Joint Institute
University of Maryland Medical Center
DISCLAIMER: The purpose of this site is purely informational in nature. It is not intended to diagnose, treat or cure any medical condition. This information is not a substitute for advice from a medical professional. Please consult your healthcare provider for accurate diagnosis and treatment. The information presented here may be subject to errors and omissions.
SITE LAST UPDATED: APRIL 2026



Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…