osteoporosis
AUTHOR: Marc Mitnick DPM home --> osteoporosisbone decalcification
Osteoporosis is a progressive disease where the bones of the body de-calcify over time thus weakening the bone itself. This weakening of bone makes it more susceptible to fracture (with or without trauma). Usually these fractures occur in the hips, spine and wrist but certainly can occur anywhere in the body including the feet.
It is estimated that over 10 million Americans have bone demineralization and many millions more have low bone mass known as osteopenia which if untreated will deteriorate to osteoporosis.
This condition is diagnosed through bone mineral density tests also known as the DXA test. Not only is this test used to make the diagnosis, but it can also check the strength of the bone tested plus it is also used to see if any treatment the patient is under going is actually strengthening the bone.
risk factors for osteoporosis
Bone loss is caused by a number of risk factors. They are further divided into factors that you can change and factors you have no control over.
Factors you cannot change:
- Gender. Women get osteoporosis more often than men.
- Age. The older you are, the greater your risk.
- Body size. Small, thin women are at greater risk.
- Ethnicity. White and Asian women are at highest risk. There is a lower risk in Black and Hispanic women.
- Family history. Tends to run in families. If a family member has this condition, then there is a greater chance that you will too.
Factors you can change:
- Sex hormones. Low estrogen levels can cause bone thinning in women as can low testosterone levels in men.
- Anorexia nervosa. This eating disorder can lead to bone loss.
- Calcium and vitamin D intake. A diet low in calcium and vitamin D makes you more prone to bone loss.
- Medication use. Some medicines increase the risk of osteoporosis.
- Activity level. Lack and exercise can weaken bones.
- Smoking. Cigarettes are bad for bones.
- Drinking alcohol. Too much alcohol can cause bone loss.
We reach our peak bone mass at around age 30, but our bones continue to remodel. Cells known as osteoclasts breakdown bone, generally old and poorly structured bone and osteoblasts are cells that come in and lay down new bone. If the amount of new bone is equal to the amount of old bone being destroyed then the bones stay strong. When this “balance” starts to favor the osteoclasts, bone starts to weaken. The drug Fosamax works by inhibiting osteoclast activity.
Bone is built in a lattice type network. Note the picture below. You will see that healthy bone bridges from one end to the other similar in structure to the steel network seen in tall office buildings. When bone loss sets in, one can readily see how the lattice network is destroyed and thus the bone becomes weak.
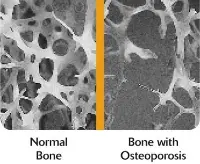
|
osteoporosis and the feet
The reason why I chose to include this subject is because of the affect it can have on the feet; not so much from a fracture standpoint as I am not even sure I have seen a foot fracture that I attributed to osteoporosis in all my years of practice but rather another ramification of the disease as it relates to foot pain.
Many older individuals will present to the office complaining of generalized foot pain, more often than not both feet are affected. The patient generally cannot pinpoint an area that hurts but rather a complaint of nondescript pain in both feet. Yes, sometimes they may suffer from multiple arthritic joints, but they usually can then point to areas of the feet that hurt.
When the complaint is of pain with vague symptoms many times it can be from osteoporosis. As the bones of the feet demineralize over time, they become weaker but are still expected to support the whole body. This weakness in the bones reduces the strength of the individual bones and it is manifested as generalized foot pain.
Look at the x-rays below. The picture on the left exhibits bone loss. The internal architecture of the bone is “washed out”, whereas the x-ray on the right is of normal bone and if you look closely you can see the normal lattice network of the bones.
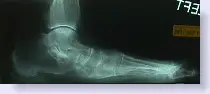
|
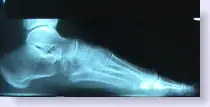
|
For the individual who already suffers from bone demineralization there is not much that can be done to reverse the condition. As far as foot pain from bone weakening is concerned, wearing good solid laced shoes with an arch support can go a long way to reducing the stress placed on the bones in an effort to support the feet.
Most experts recommend the following in treating bone demineralization (before it occurs):
- calcium supplements and increased calcium in your diet.
- vitamin D supplementation, 800 international units/day.
- eat foods rich in vitamin k (broccoli, cabbage and spinach)
- exercise in an effort to strengthen bone.
- cessation of smoking.
- moderation of alcohol consumption
- up until recently HRT, hormone replacement therapy, was advocated but it is now known that the risks of estrogen therapy far outweigh the benefits.
The suggestions above are the conventional wisdom given by most doctors today. I thought I would include an essay by Jon Barron, a world renowned leader in the field of alternative medicine. His viewpoint is different but it makes a lot of sense. Decide for yourself.
Osteoporosis
by Jon Barron (Jonbarron.org)
There's an old saying, "Insanity is doing the same thing over and over and thinking that some day the result will be different."
Now, you can argue that's also the definition of persistence as in Colonel Sanders, who was rejected by hundreds of restaurants and a thousand banks before he sold his first Kentucky Fried Chicken franchise. But when it comes to osteoporosis, it truly is the definition of insanity. Amazingly, 99% of the medical community and the media promote a solution that not only does not work, but has been proven to actually exacerbate the problem. But that's not the worst part. Even more insane is the fact that although research has shown that taking more calcium and drinking more milk actually contribute to bone demineralization and make it worse, our doctors don't just tell people to continue doing these things -- they tell us that it's not working because we're not doing enough. Therefore, we need to do even more!
What is osteoporosis?
As defined by the World Health Organization, this is a generalized skeletal disorder characterized by thinning of the bone and deterioration in its architecture, causing susceptibility to fracture. The key phrase here is "susceptibility to fracture." There are two types of osteoporosis:
Type I osteoporosis (postmenopausal osteoporosis) generally develops in women after menopause when the amount of estrogen in the body decreases. This process leads to an increase in the resorption of bone (the bones loses substance). Type 1 osteoporosis is far more common in women than in men, and typically develops between the ages of 50 and 70. The decrease in the overall strength of the bone leads primarily to wrist and spine fractures.
Type II osteoporosis (senile osteoporosis) typically happens after the age of 70 and affects women twice as frequently as men. Type II osteoporosis involves a thinning of both the hard outer bone and the spongy bone inside. This process leads to hip and spinal fractures.
Note: approximately 20% of women and 40% of men with osteoporosis have a secondary cause such as hyperthyroidism or lymphoma.
The Statistics
Osteoporosis has been recognized as a major public health problem for only the last 20 years. (In the old days, it was just called "widow's stoop.") The increasing incidence of fragility fractures, such as spinal, hip, and wrist fractures, first became apparent from epidemiological studies in the early and mid-1980s. (NWHIC) Today, approximately 10 million Americans (8 million women and 2 million men) have osteoporosis
Another 34 million show signs of low bone mass indicative of a future problem.
At the present time, the majority of hip fractures (the major danger from osteoporosis) occur in Europe and North America. In 50 years, however, it is estimated that 75% of all hip fractures will be occur in developing countries, with the numbers of hip fractures rising three-fold to 6.3 million a year.
It is now clear that the rate of increase for osteoporosis is faster than the growth in population, and it is growing in parts of the world that never showed much evidence of it previously.
The Medical Mantra
At one time, the medical mantra was that it's all hormonal. It's a woman's disease. That meant hormone replacement therapy was the answer. But as more study results came in, that theory became unsustainable -- at least by itself. It couldn't explain the dramatic increase in the incidence of osteoporosis in the United States and throughout the world, and it couldn't explain the ever increasing number of men who were becoming afflicted. So a new theory had to be developed -- the bone mineral density theory. This theory stated that people weren't getting enough calcium in their diets so they weren't able to build enough bone mineral density to serve as a reserve as they got older; thus they couldn't compensate for the natural bone loss that occurred as they aged. The obvious solution: calcium supplementation. So, according to the latest wisdom, we should:
- Drink more milk.
- Take calcium supplements.
- Use HRT (hormone replacement therapy) to rebalance hormonal levels.
- Drink fluoridated water since fluoride builds bone mass.
- Use Fosamax, the latest wonder drug to prevent the destruction of bone.
If you go to a doctor and ask about osteoporosis, 99% of them will recommend some combination of the above -- even though we now know the protocol doesn't work and in fact contributes to the condition.
Which, of course, makes us ask the question, "Why doesn't it work?"
The Reality
A number of people in the alternative health community, including myself, have argued for years that excessive calcium doesn't help the problem; it contributes to it. Magnesium is far and away the more important mineral (but still a secondary piece of the puzzle) when it comes to bone loss. I covered this in detail back in 2003 in a newsletter titled The Calcium Question, but based on the number of questions I've recently received concerning osteoporosis, it seems that most people visiting the Foundation website are not finding that newsletter. So let's cover some of the key issues again, and let's begin by quickly discussing how the body builds bones.
First, (and this may be a surprise to many people) your bones are living tissue. They are not dead cement. By living tissue, I mean that bone is comprised of living cells (osteoclasts and osteoblasts) that are continually removing and replacing the mineral deposits that we normally think of as bone. The brilliance of this system might not at first be obvious. After all, what possible advantage could there be to getting rid of good bones. Isn't that osteoporosis? And the answer is that it's only osteoporosis when we mess up the balance -- when we lose more bone than we build.
Think about this for a moment. If building and replacing bone wasn't a dynamic process, how could you mend broken bones or replace aging fragile bones? And if the process went only one way (just building bone), your body would eventually become one solid mass of bone. When you are healthy, it is this dynamic process of removing and replacing the bone minerals that keeps your skeletal system healthy -- as long as that process is in equilibrium. As with almost all diseases, it is deviation from the natural state of balance that causes problems. What do I mean by deviation? Quite simply, deviation is when we start losing bone minerals faster than we replace them. That's osteoporosis.
So what causes us to go out of balance? If you believe most of what you see and hear, it's hormonal imbalance and insufficient calcium in the diet so that we cannot grow new bone fast enough -- thus the need for calcium supplements and high dairy intake and of course, HRT. But the simple truth is: the facts don't bear this out. The incidence of hip fractures (a good indicator of osteoporosis) in countries that have the highest dairy consumption in the world (like Norway, Sweden, and the United States) is 50 times greater than in countries like New Guinea and South Africa that have extremely low consumption of dairy products (and animal products in general).
Bottom line: high calcium intake does not prevent osteoporosis -- not even among people who use coral calcium.
The simple truth is that if we live a balanced lifestyle, we actually need very little calcium (of the right sort) to maintain healthy bones. The problem we have is not that we get too little calcium, but rather that we have made choices that dramatically accelerate the rate of bone loss -- to the point that we can never consume enough calcium to overcome the deficit.
Which lead us to the question of the day: what accelerates bone loss to such a degree? And there are several answers:
- Lack of sufficient weight bearing exercise accelerates bone loss. (Thus, increasing exercise helps reverse it.)
- Insufficient boron and vitamin D3 contribute to bone loss.
- Insufficient magnesium in the diet is more of a factor than
- insufficient calcium. A study in the Journal of Nutritional Medicine, 1991; 2:165-178, for example, showed that after nine months, women on magnesium supplements increased bone density by some 11%.
- Increasing the amount of gamm linolenic acid and eicosopentacnoic acid in the diet helps increase bone density.
- Avoiding fluoride in your drinking water is vital. Fluoride collects in the bones, and although it "technically" increases bone mass and density, the evidence is very strong that fluoride intake can actually double your risk of hip fractures..
- Balancing out hormones. Does that mean that I'm recommending hormone replacement therapy? Hardly.HRT as it is practiced, doubles your risk of cancer and offers only a temporary reprieve from osteoporosis. What most people don't realize is that bone loss accelerates rapidly in women once they stop using estrogen, causing a "catch-up" effect. By age 80, women who had taken HRT for 10 years and then stopped for 10 years would lose 27 percent of their initial bone density, while those who were never treated would lose about 30 percent. The only way you would get continued benefit is take HRT for the rest of your life, which would likely be shorter because of the increased risk of developing breast and endometrial cancer. Bottom line: HRT doesn't build bone; it only slows the rate of loss and at great risk. Natural progesterone, on the other hand increases bone strength and density by stimulating osteoblasts, your bone building cells and does not carry the same risks.
- And what problems do I have with Fosamax? Other than the fact that it works by totally destroying the bone building process, not much. Quite simply, it works by killing osteoclasts. As we discussed earlier, these are the cells that remove old bone so your osteoblasts can build new bone in its place. Well yes, if you kill off the osteoclasts, your bones are going to get denser because instead of replacing old bone, the new bone will "cram" itself into whatever space it can find. Unfortunately, this also means that your bones are going to get weaker because you're not eliminating the older damaged bone. Fosamax builds a house of cards that must ultimately collapse.
But all of the above factors pale in comparison to the problem of a high acid diet. This is the reason the incidence of osteoporosis has soared. This is the reason more and more men are now suffering. If you have not already done so, I suggest you read Chapter 13 of Lessons from the Miracle Doctors (you can download a free copy at www.jonbarron.org/books.php> ) to better understand how a high acid diet (meat, fish, poultry, eggs, dairy, cooked grains, and refined sugars) leeches calcium from the body. The brief explanation is that when you consume a high acid diet, your body is forced to use calcium from your bones to buffer the high acid content so that your blood pH remains constant and you don't die. The problem with dairy is that it actually takes more calcium to buffer its acid content then you actually receive from the dairy -- thus the high incidence of osteoporosis in countries that consume a lot of dairy. Now, do not misunderstand. I am not saying that dairy is the biggest culprit. Actually, all of the other acid foods are worse -- particularly high sugar colas. I just single out dairy because it's always identified as building strong bones, when the opposite is true.
So what is one to do? Well, first read Chapter 6 of Miracle Doctors. It lays out the ground rules for a diet that allows your body to build bone. It suggests minimizing the intake of animal foods (to less than 3 ounces a day) and the elimination of refined grains and sugars. At that point, the amount of highly absorbable calcium that you get in your diet from foods such as romaine lettuce, broccoli, sesame seeds and bok choy will be more than adequate to build strong bones.
Think about cows for a moment. (This is one of those questions that I love to use when I want to drive doctors crazy -- a hobby of mine.) How do cows grow such large, strong bones? They don't drink milk, and they don't take calcium supplements. They eat grass -- low in calcium, high in magnesium (magnesium is the basis of chlorophyll in plants). Consider the fact that the traditional Eskimo diet contains over 2,000 mg of calcium a day, but because their diet is so acidic (virtually 100% from animal sources), it produces the highest hip fracture rate in the world. The bottom line is that calcium supplementation will not save you from the consequences of a high acid forming diet.
And if you absolutely can't change to a more alkaline diet, then taking supplemental calcium (not milk) to buffer the excess acid probably makes sense. It won't repair any damage, but it will protect against some of the destruction you are inflicting on yourself.
December 2006. Reprinted by permission
REFERENCES


Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…