athletes foot
AUTHOR: Marc Mitnick DPM
REVIEWED BY: Podiatric Medical Review Board
home --> athletes foot
WHAT IS ATHLETES FOOT
This is a common fungal infection of the foot. It is estimated that upwards of 70 percent of the population will suffer from this condition sometime during their life. Athletes foot does not necessarily only affect physically active individuals; it can occur anytime conditions are right; usually dark moist environments is where this type of fungus flourishes.
This condition is also known as a superficial dermatophyte meaning it grows in the superficial layers of skin. There are four dermatophytes that can cause this condition, also known as tinea pedis and ringworm of the foot. The most common is trichophyton rubrum.
ATHLETES FOOT SYMPTOMS
Actual foot fungus will manifest itself in different ways.
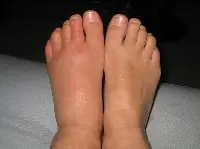
ACUTE TYPE The most painful, is an annoying persistent itching of the skin on the sole of the foot or in between the toes. As the infection progresses, the skin grows soft. The center of the infection is inflamed and sensitive to the touch. Gradually, the edges of the infected area become milky white and the skin begins to peel. There may also be a slight watery discharge. Although this condition can be very uncomfortable in terms of itching, the bigger problem is the formation of a secondary bacterial infection, where bacteria enters the opening in the skin created by the fungus, and a resulting cellulitis.
|
The secondary bacterial infection is potentially a much more dangerous condition, particularly in diabetes and those with suppressed immune systems.
Note the left foot in this picture. The redness seen around the toes is a secondary cellulitis from an existing fungus infection in between the toes. Not only did this patient require treatment for the fungus infection but also oral antibiotics for the cellulitis.
CHRONIC TYPE This is characterized as a non-inflammatory type of athletes foot.

|
Many people will present to the office complaining of chronic dry skin particularly in their heels, although it is also seen around the ends of the toes. They have tried different dry skin lotions with no success. What they fail to realize is that part of that “dry skin” component in the heel and toes is actually chronic athletes foot and unless that issue is addressed, the heels will not clear up. (See my section on heel fissures)
Another problem with fungus infections of the skin is that it can spread to the nails of the feet and then infect them. This condition is known as onychomycosis. The reverse is also true. In those individuals that suffer from mycotic nails it is not uncommon to see the condition spread to the skin in the form of skin fungus.
Depending on its presentation skin fungus at times can be difficult to distinguish from eczema. Topical cortisone cream is generally used for eczema; if it is used on athletes foot, it will suppress the symptoms of athletes foot but usually the fungus will worsen once you stop using the cream. Other skin conditions that mimic athletes foot include contact dermatitis and psoriasis.
DIAGNOSING ATHLETES FOOT
Most cases of athletes foot can be diagnosed on clinical examination. Combining that with a good patient history.
- do the feet perspire
- is the patient athletic and spends a lot of time in locker rooms
- does the patient wear closed shoes and moisture retaining socks/stockings for long periods of time
- in some cases, a suppressed immune system can be a factor
- diabetics have a higher incidence of fungus infections
- positive family history
ATHLETES FOOT TREATMENT AND PREVENTION
how to get rid of athletes foot
The best way to suppress this condition is to eliminate the environment in which it flourishes. As previously mentioned, fungus thrives in dark moist environments, so by reversing that environment you can better control the condition.
This means alternating your shoes on a daily basis.
It also means allowing your shoes to “air out” by not throwing them in a dark closet at the end of the day but perhaps keeping them by an open window or back porch in an effort to allow them to dry out.
Spray the inside of the shoes with an anti-fungal spray.
Wearing perspiration absorbing socks and perhaps even changing them twice a day can be very beneficial especially in severe cases. Socks with impregnated silver in them are thought to be anti-fungal and anti-bacterial.
When bathing, wash the affected area well with tea tree oil soap and water and then dry the area well. I recommend tea tree oil soap over bar soap because of the anti-fungal properties found in tea tree oil soap.
Avoid commonly shared surfaces such as bathrooms, gyms and pools where it is very easily to catch or spread a fungal infection.
Avoid scratching the area as this will make the symptoms worse, increase the chance of a secondary bacterial infection and spread of the fungus to other parts of the body.
athletes foot remedies
Most of the prescription anti-fungal medications are now sold over the counter. The biggest mistake people make is not using the medication for a long enough period of time. As the condition begins to improve many people will stop using the medication thinking the condition has resolved. Unfortunately the fungus is still residing in the skin and in many cases the symptoms will return. In most cases topical anti-fungal cream has to be used twice a day for 4-6 weeks regardless of how good the foot may look or feel.
For those who have feet that perspire quite a bit, use of a topical drying agent can be very helpful. Two such products are Bromilotion by Gordon Labs and Onox spray, both of which can be purchased on Amazon.com.
In severe cases, that do not respond to the above suggestions, oral medication such as Lamisil, Sporonox and Griseofulvin may be used for short term doses. The major side effect of these medications in short doses is stomach irritation.
For those individuals who are prone to fungus infections of the foot such as people who work in warm moist environments, those who must wear high top work boots and athletic individuals, foot fungus will be an ongoing problem with recurrences, but by following the advice given above you can minimize its recurrence and its symptoms.
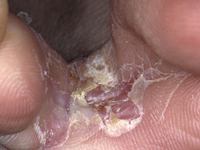
athletes foot image
 |
REFERENCES
American Academy of Dermatology
Want more information? CLICK HERE
Para traducir esta pagina, ve al boton de traduccion de Google en las esquina superior derecha de la pagina


Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…