bunions
AUTHOR: Marc Mitnick DPM home --> bunionshallux valgus and tailors bunion
WHAT IS A BUNION
Otherwise known as hallux valgus, this is a deformity of the big toe joint. This type of pathology is usually manifested as a bump on the inside of the foot just behind the big toe. The bump can be very small or reasonably large; the size of which is not necessarily proportional to the amount of pain one can experience. Along with this bony bump there can be an associated bursitis which is a “cushion” that the body originally creates to protect an area from pressure or friction, but after a while this cushion can also become inflamed and painful. The last component of this deformity is the deviation of the big toe as it moves toward the second toe, sometimes even underlapping or overlapping the second toe.
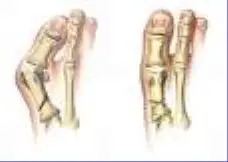
Here is a skeletal representation of a big toe joint deformity on the left, compared to a normal foot on the right.
|
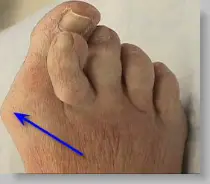
What does a bunion look like? Below is a hallux valgus deformity (blue arrow) with the big toe under lapping the second toe.
|
WHAT CAUSES BUNIONS
Poor fitting and high style shoes are usually blamed as the culprit for the formation of this deformity, that is why they are more prevalent in women.
But, is that really what causes bunions?
Inherited foot structure-The truth is most of these deformities are based on a particular foot structure and the way a person walks. This is one of the reasons you can see this development in children who typically wear very conservative shoes.
The biomechanics behind hallux valgus formation-The short story is feet that have a tendency to excessively pronate cause an over-flattening of the foot.
- This excessive flattening causes excessive tension on the extensor hallucis longus tendon (the tendon on the top of the foot that enables you to bend your big toe upwards).
- This causes the tendon to "bowstring".
- In doing so forces the big toe to be pulled laterally, toward the second toe. This is what causes the initial deviation.
- Over time, there is a retrograde (or backward) force placed on the first metatarsal bone by the big toe.
- The first metatarsal bone begins to move medially (or away from the second metatarsal bone).
- Due to these changes there is now more pressure on the side of first metatarsal bone from shoe pressure and this causes a hyperostosis or thickening of bone and this results in the bump, that you see and feel on the inside of the foot.
This deformity also creates an unequal alignment of the joint itself and causes the joint to wear out, over time. Once the joint is worn down sufficiently pain ensues when you try to bend the toe while walking.
So, the biomechanics of the foot is really what causes bunions.
In theory, if you lived on a tropical island and never wore shoes your whole life, you could still develop hallux valgus.
Below is a video describing what causes bunions in technical detail.
Generally speaking, hallux valgus is a progressive deformity and in most people will worsen over time (if appropriate measures are not taken to remove the underlying cause).
HALLUX VALGUS SYMPTOMS
BURSITIS-The most common pain associated with hallux valgus is the pain that occurs from the inflamed bursal sac, also known as an inflamed bunion. Typically, there will be a burning sensation in that area of the foot. Inspection will reveal swelling and redness. This can occur even with very small bumps on the side of the foot. Shoes, particularly women's dress shoes create a lot of pressure against the bone and the body's reaction to that is to form a bursal sac which initially is designed to protect the area, but invariably, will become inflamed and begin to hurt. Whenever, I do bunion surgery, I always look for, and have removed inflamed bursal sacs.
BUMP PAIN-Even without a bursitis, the bony bump can become painful, again usually aggravated by dress shoes, but in many individuals, even conservative shoes like sneakers will cause pain. The size of the bump and the activity level of the patient are two factors that will lead to bump pain. In this instance there does not necessarily have to be swelling and redness. This pain is usually only evident when wearing shoes and will vary with the type of shoe being worn.
JOINT PAIN-The other type of pain in this condition is what is known as joint pain. As the big toe starts to move closer to the second toe it creates an abnormal alignment in the big toe joint. This causes a premature erosion of cartilage and over time the joint will no longer move smoothly and the patient will start to experience pain and limitation of motion of the big toe. This type of pain can be experienced both in and out of shoes.
TREATMENT AND PREVENTION
Just because you have this deformity does not necessarily mean you have to have treatment. In the asymptomatic or non-painful deformity it is more prudent to find the underlying cause of the deformity and make changes accordingly.
Having said that, I can tell you that over the years I have had patients come to me with what appears like a golf ball growing on the inside of their foot and they swear to me that it does not hurt. If that is the case, leave it alone.
NON SURGICAL BUNION TREATMENT
Orthotics-So what an orthotic does in these cases is to reduce the over flattening of the foot which then results in an improved alignment of the joint and reduction of pain in the joint itself. The degree of relief is probably inversely proportional to the degree of damage that is already done. This means orthotics generally will work on mild to moderate bunion pain but not severe pain. Keep in mind that orthotics especially in women will require a wider if not slightly longer shoe. So if a shoe that is tight and irritating a bunion to begin with has an orthotic added to it, the shoe becomes even tighter (and more painful).
This therapy will not make the existing deformity disappear, but it should slow down or eliminate further worsening of the condition. Follow this link for more information, hallux valgus and orthotics.
Sensible shoes-Elimination of shoes that are either too narrow, to flimsy in support, or too high in the heel. Trying to wear a narrow high style shoe with a large great toe deformity is like trying to put a square peg into a round hole; it just does not fit. This kind of mentality will eventually lead to a worsening of the condition.
do bunion splints work?
Cushions, braces and splints-that are sold for this condition are not my first choice because in most cases they just take up more space in the shoe and put more pressure on the bump. My only exception to this is in people who are experiencing "joint pain". The best bunion splint therefore, is one worn at night that will keep the toe straight but not create excessive pressure within the shoe.
I have also been known to use these splints after surgery, for a short time, in an effort to keep the joint properly aligned during the healing process. The splint on the left is for night use only, while the splint on the right is for day time use. Keep in mind, you can only wear laced casual shoes.
AGGRESSIVE TREATMENTS
Anti-inflammatory medication-is fine for short term use but should never be considered as a solution in that over the long haul the medication will lead to systemic problems in most individuals.
Cortisone injections-can be very helpful in those have bursitis pain and to a lesser extent for those suffering from joint pain.
Physical therapy-can be helpful in relieving flare ups.
SURGERY
The question frequently asked of me is when to have surgery to correct this deformity. (It is estimated that over 200,000 people per year have hallux valgus surgery in the United States) My criteria is simple; when the pain of the deformity starts to affect your everyday life on a regular basis. You no longer golf, or go for daily walks, or go shopping with your friends out of fear that “my foot will start hurting”. Now the quality of your life is being affected. See my essay on surgical consideration.
Having said that, keep in mind that hallux valgus surgery is not without risks (as is any kind of surgery) and that the type of surgery your friend may have had, may not be the type you will require. The well trained podiatrist probably does at least a half dozen different types of procedures based primarily on the size of deformity. The type of procedure will usually determine the length of recuperation. The risks of hallux valgus surgery include the following:
- infection- (true in all types of surgery).
- loss of motion- (joint stiffness); the big toe does not bend, although in some procedures this is expected and the joint will no longer hurt.
- delayed healing- because of the dependent nature of the foot there is usually more swelling than in other parts of the body so healing may take longer.
- surgical failure- whereby you are no better off after surgery than you were before the procedure.
- nonunion- in procedures where the metatarsal bone has to be broken and re-set in an effort to re-angulate the bone, there is always the possibility that the broken bone will not heal.
- implant failure- in the case of a joint implant there is always the possibility it may have to be removed due to infection or reaction to the materials of the implant.
- recurrence of the deformity.
|
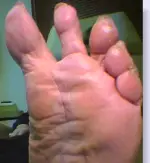
Think complications can't happen? This is a picture of an over-corrected bunion deformity; what is known as hallux varus. In an effort to move the big toe away from the second toe, the surgeon (someone else), moved the big toe too far in the opposite direction. Now the patient has even more trouble finding comfortable shoes and needless to say is quite unhappy with the appearance of her foot.
Even worse, the hallux varus throws off the "architecture" of the foot. Because the big toe and to a lesser extent, the second toe are in a "varus" position she has developed a painful corn on the end of her third toe.
The type of anesthesia used in this type of surgery ranges anywhere from local anesthesia where just the foot is put to sleep, to intravenous sedation (twilight sedation) with local anesthesia, to general anesthesia. The vast majority of my patients are done under local anesthesia with intravenous sedation on an outpatient basis. I prefer this type of anesthesia because the patient feels no pain, is not having general anesthesia and all the potential risks associated with general anesthesia, and tends to be awake shortly after surgery with less chance of being "sick" from the anesthesia during the following 24 hours.
Hallux valgus surgery has become very sophisticated surgery; it is not just a question of removing the bump. Most of the procedures done attempt to realign the joint.(joint pain vs. bump pain) Discuss your surgical options with your doctor
CRITERIA FOR CHOOSING THE PROPER BUNION PROCEDURE
Once the decision is made to have a bunion surgically corrected it now falls upon the surgeon to determine the type of procedure to be performed. Not all deformities are the same; that is essentially why one's surgical experience will probably differ from the next person.
When determining the type of procedure to be performed it is important to determine if the patient is having just bump pain, or just joint pain, or both as that will come into play in the decision process as to the type of procedure to be performed. Next, the surgeon will look at the various angles that are formed between the bones of the foot on x-ray. The accepted practice is to measure these bone angles which will help determine the type of procedure to be performed. There are easily a few dozen different procedures (and their variations) out there to repair bunions. The decision as to which one to choose many times is based on the angles that are measured on the x-ray. (I cannot emphatically state that all doctors take the time to actually draw out these angles because there is a margin of error based on the position of the foot when the x-ray was taken and the actual accuracy of bisecting the bones in order to draw out the bunion angles).
|
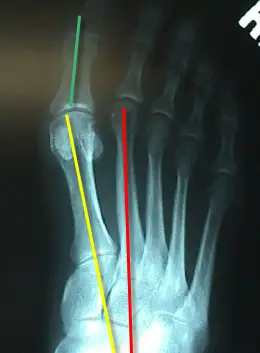
Look at the x-ray of a bunion to the right. These are two of the most common angles drawn out to evaluate which procedure to perform. (there are additional angles that may be taken into account based on the architecture of the foot in question). The angle formed between the yellow and red line is known as the intermetatarsal angle. Normal is considered 8-10 degrees for this angle. As bunions progress, this angle actually widens. The first metatarsal bone actually moves away from the second metatarsal bone. Depending on how wide the angle is at the time of surgery various procedures are available to reduce this angle. If you do not reduce this angle sufficiently, there may still be problems with the bunion after just the "bump" is removed. In general, the wider the angle, the greater the amount of work that has to be done to reduce the angle.

|
The video just below is that of an Austin bunionectomy, which is used to reduce a moderate intermetatarsal angle. This procedure is done at the level of the neck of the metatarsal. Larger angles may be reduced by doing procedures further back on the first metatarsal or even the joint just behind the first metatarsal bone. In general, one will be able to ambulate after a simple bunionectomy (just having the bump removed with a normal intermetatarsal angle, or even with a procedure done at the neck of the metatarsal such as the Austin, but procedures done further back will usually require a time period of being non-weightbearing.
The angle formed between the yellow and green line represents the hallux abductus angle or the deviation of the big toe (hallux) relative to the first metatarsal bones. If this angle is too large there are osteotomy procedures available (surgically breaking and re-aligning bone) to fix this angle as well.
Not only are the angles that form the bunion important, but the actual condition of the joint itself is also very important. If the cartilage making up the joint is too far eroded then even a procedure that creates perfect alignment of the joint is still going to be problematic for the patient. It is at this point that the surgeon has to decide to either remodel the joint or replace the joint with an implant or artificial joint. Unfortunately, the only real way to know the actual condition of the joint is to visually inspect it, once the foot is open. In general older individuals who also happen to be more sedentary are better candidates for great toe joint implants because quite frankly there is a life expectancy to implants meaning they can and do wear out over time.
Here is a video of an Austin bunion surgery. The metatarsal bone is surgically broken with precise cuts in an effort to realign the bone (osteotomy). With the great fixation procedures that we have today people can walk after this bunion osteotomy.
As a side note new advances in medicine seem to be occurring on a daily basis. Bunion surgery is no different. The video you just viewed of an Austin bunionectomy shows one of the procedures we do to surgically break and reset bone (osteotomy) in an effort to move the first metatarsal bone closer to the second metatarsal bone to get better alignment of the big toe joint.
A new device called the TightRope fixation manufactured by Arthrex is a high tension wire that is placed through the first and second metatarsal bones in an effort to reduce the distance between the two bones. The beauty of this concept is that an osteotomy does not have to be performed. Since most bunion complications generally center around the osteotomy itself, having another option to reduce the intermetatarsal angle is very exciting.
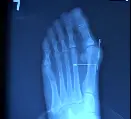
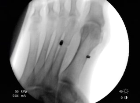
If you look at the two x-rays below the one on the left is the preoperative x-ray. The goal of surgery as represented by the horizontal arrow is to move the first metatarsal bone closer to the second metatarsal. The x-ray on the right is the postoperative view and you can see the "tightrope" that has been drilled through both the first and second metatarsal bones and is held together by the black anchors.
I must caution you that the use of the TightRope for bunion correction is a relatively new concept but is very promising.
Update November 2010 After having read a recent study regarding the TightRope procedure I thought I would pass along some of the findings. Please keep in mind this was a very small study and it was done on people who had the procedure performed two years ago or less. (This procedure, like most medical procedures need to be examined at least five years down the road with a large patient population.)
The most common complication from this type of procedure has been fracturing of the second metatarsal bone which in all cases required further surgery to correct the fracture. There are a number of reasons this may happen. If the bone stock is not adequate, meaning there is a reasonable amount of osteoporosis or osteopenia, whereby the overall calcification is diminished. Of course this is a problem that should be looked at pre-operatively in any potential candidate. Secondly, one also needs to evaluate the overall thickness of the second metatarsal bone. Many people exhibit a very thin second metatarsal bone relative to the first metatarsal and to expect the thinner bone to support the larger bone may be a bit of a stretch. This too should be evaluated pre-operatively.
The study mentions other possible causes for failure such as the fact that the drill holes through the second metatarsal bone will naturally weaken the bone. In addition they mention the fact that the first metatarsal bone has its own range of motion independent from the other metatarsal bones, thus putting more stress on the second metatarsal bone. Exacerbating the problem is the fact that the tension wire itself is made of a hard abrasive suturing material that over time in connection with the movement of the first metatarsal will cause a "sawing" motion on the second metatarsal and will eventually weaken the bone.
If any of you reading this section are contemplating having this procedure done, please discuss these potential complications with your surgeon.
|
|
Update June 2016 In an effort to refine the tightRope procedure, other companies have come out with different variations of the hardware used for this type of correction. One company, Arthrosurface, has come out with a device known as the KISSloc Suspensory Suture System.
|
The next video demonstrates implant surgery for correction of a bunion. As just mentioned, this is generally done when your doctor determines that the cartilage is too worn out to be salvaged and is then replaced by an artificial joint. This procedure is sometimes performed in conjunction with an osteotomy procedure to realign the metatarsal and toe bones.
Many patients ask me if you can have laser surgery on bunions. The answer is no. Theoretically you could use a co2 laser to make the skin incision (which I have done) but it really affords no advantage over a regular scalpel incision. More importantly, lasers cannot remove bone, all they do is burn bone, so a laser could not be used to remove the large bump of a bunion deformity.
minimally invasive bunion surgery
For those individuals that have a painful bump on the inside of the foot and the angle between the first and second metatarsals is essentially normal, many times just the "bump" can be removed through a very small incision. Using a high powered burr, the enlarged bone can be burred away resulting in an elimination of the bony protrusion. The problem I have always had with this procedure is that in the process of burring away excess bone, the surrounding soft tissue structures, primarily the capsular and collateral ligaments will also be destroyed. Destruction to these ligaments may adversely affect the function of the big toe joint in the future.RECOVERY FROM BUNION SURGERY
what to expect after bunion surgery
Recovery time after bunion surgery will vary depending on a number of factors.
Probably the most important factor is the type of bunion surgery performed. People will generally recover quicker with a more simpler procedure. The more complicated procedures take longer to heal, then there is also the time period afterwards to rehabilitate the joint generally through physical therapy. This does not mean you are not walking after bunion surgery; in most cases the patient is walking immediately. By this I mean you can ambulate from day one (there are some bunion procedures where you have to be nonweightbearing for a period of time; discuss this with your doctor), meaning you will be able to get around and take care of yourself but by no means will you be on the golf course.
In an otherwise healthy individual who has undergone an osteotomy (surgical breaking and re-alignment) for their bunion deformity, in most cases it will take 6-8 weeks for the surgical site to completely heal. Virtually all osteotomies are fixated with hardware such as screws, plates, k-wires, wire suture, etc. to keep the alignment in position. So even if your surgeon allows you to bear weight and walk on your foot it will be with limitations until the fracture has completely healed.
In simpler bunion procedures where there are no bones surgically broken and in cases of implants for the great toe joint, the current thinking is to get the patient walking as soon as possible in an effort to exercise the joint and reduce the possibility of joint stiffness which in itself can become an issue.
Other factors that will affect the recovery time after bunion surgery include your age, younger people tend to heal quicker, your overall health, and maybe the most important factor is patient compliance. Follow your doctor's postoperative orders for home care and mobilization. Generally, when patients are noncompliant they will run into more postoperative problems.
Time of year-As previously mentioned, because of the dependent nature of feet, they tend to swell in hot weather. The older you are, the more they swell. Foot surgery also causes feet to swell simply because the body's way of healing an injured area is to increase the blood flow to the area bringing with it nutrients that facilitate healing.
So, if you have foot surgery in hot weather, the combination of the surgery and heat may keep your foot swollen for a longer period to time then if you had your surgery in cooler weather. The time of year should not be your sole criteria for when to have surgery, but it certainly should be part of the decision making process.
exercise after bunion surgery
The two general questions I am usually asked by patients is "when can I return to sports?" and in the case of women, "when can I start wearing heels?". There is no clear cut answer to these questions since every one heals at a different rate. If your surgeon is an experienced surgeon, he or she will be able to give you guidance in answer to your questions.
The goal in this day and age is to get our patients walking as soon as possible in an effort to keep the newly remodeled joint moving. Years ago the thinking was to keep the patient in bed so that the joint could heal; the problem with that line of logic was that the joint tended to get stiff and it would take even longer to rehabilitate. So, essentially, you will be exercising the bunion joint fairly quickly after surgery, but as far as returning to exercising, that decision should be left to your surgeon.
There is some controversy in the medical community about the benefit of physical therapy after surgery. I do not send all my patients for physical therapy; in fact in many cases I will just give them instructions in exercises and other things they can do at home to facilitate their healing (and only hope they actually follow my instructions).
Most experienced surgeons can get a "feel" for when a patient is not progressing along a normal healing time line. In those instances and in situations where a patient may develop a problem, physical therapy by a physical therapist becomes more important.
Once your sutures have been removed and if not in a cast, you will be ready for a shoe. This does not mean your everyday shoes. Some doctors like to have their patients wear a daytime bunion splint to maintain their surgical correction. This plus the fact that your foot will be swollen (a normal part of healing) will make it impossible to wear the shoes you already own. I generally have my patients buy an inexpensive pair of sneakers large enough to accommodate the enlarged foot and splint; this seems to work out well. If you were given a surgical shoe to wear you want to get out of that for two reasons. One, it limits motion in the joint, which we do not want and secondly patients start complaining of back pain, plus, you cannot drive with a surgical shoe if it is on your right foot.
One of the newest bunion procedures being performed today is the Lapiplasty procedure. It is a novel approach to an older technique where the correction of the bunion is made at the level of the metatarsal cuneiform joint. It is done in such a manner to a yield a more stable correction, thus increasing the chance of a positive outcome. Review the video below.
Para traducir esta pagina, ve al boton de traduccion de Google en las esquina superior derecha de la pagina
TAILORS BUNION
While we are on the subject of bunions we should also discuss the condition known as tailors bunion. This is a bunion deformity on the outside of the foot, sometime referred to as a fifth metatarsal bunion.
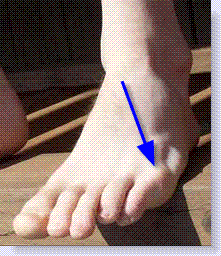
In the picture below you will notice the location of a tailors bunion.
|
This condition got its name from the turn of the last century when tailors would spend long hours working with their feet crossed in such a manner that the outside of the feet would continually press against the floor and as a result, over time, the bump on the outside of the foot would form.
This condition can be an acquired problem such as the example above or a congenital problem where there is a flare laterally of the fifth metatarsal bone resulting in the head of the bone being very prominent.
In either case the foot now has trouble fitting into a conventional shoe, (it is too wide). If there is enough pressure on the bone a secondary bursitis may form which will make the pain even worse. In those with poor circulation the skin overlying the bone may breakdown from too much pressure.
A tailors bunion will generally only hurt in shoes and be fine barefoot, or in open shoes like a sandal.
So now that we know the major precipitating factor is shoes, the sensible move would be to avoid shoes that aggravate the condition. Shoes that are too narrow, or have too high a heel, or are made of very stiff material will all go a long way to aggravating the tailors bunion.
You can always try padding over the tailors bunion but I generally find that to be a waste of time. All the pad does is take up more room and cause the tailors bunion to hurt more.If there is an inflamed bursal sac, a cortisone injection can be very helpful with the understanding that if you do not modify your shoe selection, the problem will eventually return.
Anti-inflammatory medication can be tried but I find it is rarely helpful by itself.
If all else fails there is always surgical intervention. A tailors bunion is different than the classic bunion in that in this type of bunion we do not really have to worry about biomechanical considerations.
Sometimes going in and removing the enlarged bone is all that is necessary, but in general, if there is a real lateral flare to the fifth metatarsal bone, an osteotomy (cutting and resetting of the bone to change its angulation) may be necessary.
REFERENCES
Want more information? CLICK HERE


Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…