decubitus ulcer
AUTHOR: Marc Mitnick DPM home --> decubitus ulcerWHAT IS A DECUBITUS ULCER
A decubitus ulcer otherwise known as bed sores or pressure sores occur when there is excessive pressure on skin, underlying muscle and bone for prolonged periods of time. The poorer the circulation is to the affected area, the greater the likelihood of an ulcer forming. Pressure and friction at the site may cause circulatory embarrassment to the area resulting in a reduction of oxygen to the affected tissue and from there the skin and underlying structures begin to breakdown.
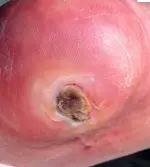
Irreversible damage may occur in as little as 2 hours of continuous pressure. Although the skin can withstand the negative affects of direct pressure, usually it is the underlying muscle that begins to deteriorate due to the higher oxygen requirements of muscle and so damage may actually occur to the muscle before it is even noticed in the skin.
Reduced mobility and lack of sensation predispose the patient to this condition and of course it is the direct uninterrupted pressure that ultimately causes the breakdown of tissue. For this reason, every patient with limitation of motion and diminished sensitivity is a potential candidate for a decubitus ulcer.
Patients at risk include:
- those who are bedridden or have limited mobility
- those with neurological disease
- those on medications that diminish sensation capacity
- those who are malnourished
- those with poor circulation to the affected area
- smokers
- diabetics
- those with collagen diseases such as rheumatoid arthritis which can result in contractures that put excessive pressure on joints
- those that have been on corticosteroids for long periods of time
- malignancies
- those wearing a poor fitting cast
- those exposed to long periods of cold
Preventable measures for decubitus ulcer requires eliminating or reversing any of the above factors.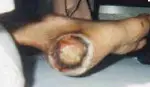
According to an article in the 2008 edition of "Wound Repair and Regeneration" the prevalence of decubitus ulcers in hospitalized patients has ranged between 14 to 21 percent. The costs associated with healing these wounds has soared as well and the truth of the matter is that by and large these are preventable complications.
Decubitus ulcers may appear anywhere on the body where there is excessive pressure, but one of the most common areas are the feet, particularly the heels.
TREATMENT FOR DECUBITUS ULCER
Treatment of bed sores is two fold in nature.

The first is to eliminate the excessive pressure.
In the feet that is accomplished by off loading where the foot may be slightly elevated off the bed through the use of various devices to lift the legs slightly. Additionally, there are various types of heel cushions that allow the foot to touch the bed without creating excessive pressure on the heel area. A key component is to make sure that by off loading one foot, you do not create excessive pressure on the other foot or any other part of the body for that matter. Without resolving the pressure issue, the ulcer will never heal. An important point to remember is that pressure sores in the foot do not always have to occur from being bedridden; sometimes very poor fitting shoes, worn on a regular basis will also cause decubitus ulcers.
The second is the actual treatment of the ulcer.
In those that are malnourished increasing caloric intake and protein may go a long way to improving outcomes.
The proper way to assess a bed sore is to look at it from various standpoints. How wide is it? How deep is it? Does the wound appear to be infected? What does the base of the ulcer look like; is it vascularized enough to actually heal? Keep in mind that even wounds that are not infected tend to have drainage coming from them. Your doctor will assess the base of the wound to determine what structures are involved, how deep the wound is and what is the vitality of tissue; in other words does the wound have the ability to heal.

stages of a decubitus ulcer
Decubitus ulcers are generally classified by the amount of tissue damage. Early signs of a decubitus ulcer may show nothing more then a discoloration in the pressure area. In the foot this is usually the back of the heel.
For example a Stage 0 wound may not exhibit any discontinuity in the skin (the skin has not broken down) but may have a bluish-purple color to it or may even have a blister which tells your doctor that there is trouble brewing. The ulcer classification ranges all the way up to Stage 4 which means the skin is completely obliterated and muscle, tendon or bone may be visible. It is important to note that some decubitus ulcers are so severe that they cannot be staged.
Treatment of course is predicated by the Stage of the wound. Included in the thought process that goes into treating the wound is whether or not the ulcer is infected which may require antibiotic therapy or at the very least a topical antibiotic cream such as Silvadene which is a silver based cream that has been shown to destroy bacteria.
If the ulcer contains necrotic tissue (dead infected tissue) that will have to be debrided (removed) by your doctor. Dead tissue harbors bacteria and is an obstacle to healing the wound.
Debridement is accomplished in a variety of ways:
- use of a scalpel to cut the dead tissue away, however, this can be very painful to the patient. Sometimes, this is done in the operating room under anesthesia.
- topical creams known as enzymatic debriding creams, such as Santyl Collagenase, which will actually dissolve necrotic tissue. They are generally used in those patients where surgical debridement is not an option.
- the use of "wet to dry" dressings where the dressing over the wound is saturated, generally with saline and allowed to dry. Once dry, the dressing can be removed and with its removal will usually take off the necrotic tissue with it. Care must be taken in removing the dressing.
- wound irrigation where the ulcer is "sprayed" with saline under a mild degree of pressure.
- whirlpool treatments attempt to accomplish the same thing as the wet to dry dressing.
Sometimes the ulcer may exhibit an eschar or scab which the body actually forms to protect the area. Generally this is not removed unless your doctor suspects the underneath wound is infected.
The goal of local wound care is to create an "ideal" healing environment. That is why infections must be cleared up. Devitalized tissue (necrotic tissue) must be removed as it increases the chance of infection if left alone. Through years of research it has been determined that a moist wound creates the best environment for the ulcer to heal. However, if your doctor notes that there is too much drainage, steps may be taken through wound care dressings to decrease the drainage to an acceptable level.
In the more complicated decubitus ulcers where bone is exposed there is always the chance of an osteomyelitis. This complication may or may not be treated with antibiotics alone. In many cases this will require a combination of antibiotics and surgery where the diseased portion of bone is removed.
Because of the poor consistency of the skin in these wounds, when surgery is required they cannot be closed by simply suturing the skin back together. Usually a skin graft of some sort will be required.
In all decubitus ulcers ultimately the driving force behind treatment is the progress of the wound in healing. Slow healing of a wound (and this occurs frequently) may dictate a change in strategy. This has to be weighed against the overall health and needs of the patient.
The best way to treat a decubitus ulcer? Prevention!
REFERENCES
see related article...wound care
Want more information? CLICK HERE


Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…