hallux limitus
AUTHOR: Marc Mitnick DPMREVIEWED BY: Podiatric Medical Review Board
home --> hallux limitus
hallux rigidus or dorsal bunion
WHAT IS HALLUX LIMITUS
hallux rigidus and hallux limitus
This condition is commonly known as a dorsal bunion. This is seen as a bump on the top of the joint where bunions are commonly found. In this condition the patient is unable to fully dorsiflex (bend upwards) his/her big toe. Pain is usually, but not always, associated with this deformity. In many instances, over time, the joint will become totally immobile and the condition is then known as hallux rigidus. Interestingly enough many painful cases of hallux limitus become asymptomatic when (and if) the joint finally fuses and no longer moves.
Most authorities states that the big toe requires from 60 to 80 degrees of dorsiflexion in normal gait. Many people can get away with less than that due to compensation mechanisms in their foot function.
WHAT CAUSES HALLUX LIMITUS
- Repetitive micro trauma- For most people the cause of hallux limitus is repetitive micro trauma where the big toe is constantly jamming into the first metatarsal bone.
- Trauma- to the joint by dropping something on it or falling down.
- Gout attacks- Repeated gout attacks over time, will cause damage to the joint.
- Excessively long or short first metatarsal- The length of the metatarsal bone can affect the ability of the big toe to move upwards.
- Dorsiflexed first metatarsal bone- An elevated first metatarsal does not allow the toe to bend up over it.
- pronation
In most cases this is a progressive deformity where the patient will relate that the pain initially started as a dull ache which was transient in nature but has progressed to the point where the joint is now painful on a regular basis both in and out of shoes.
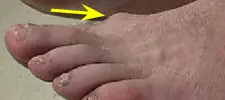
Look at the two pictures below. The one on the left is a picture of the dorsal bump. Many times the bump will be red and swollen. The picture to the right is an x-ray coming in from the side of the foot. The yellow arrow shows the excessive bone overgrowth that is occurring on top of the foot. Basically as the patient walks the big toe is unable to fully bend upwards because the toe jams into the bony overgrowth and is prohibited from moving any further upwards.
|

|
TREATMENT FOR HALLUX LIMITUS
Hallux limitus and hallux rigidus can be treated both conservatively and surgically.
Conservative options
- Anti-inflammatory medication- short doses over a period of a couple of weeks in an effort to quiet down the inflammation. This should be regarded as a temporary measure and not a long term solution.
- Cortisone injections- may be of use for short and moderate time period relief. Depending on the effectiveness multiple injections can be performed but there is a limit as to how much cortisone can be injected in the same area in a one year period.
- Physical therapy- may also be helpful in reducing the inflammation occurring in the joint. This can be combined with anti-inflammatory medication or cortisone injections.
- Orthotic therapy- an orthotic may help stabilize the joint with the addition of a Morton’s extension for hallux limitus. This is an extension that runs under the first metatarsal bone and big toe. Its purpose is to stabilize the big toe joint and thus reduce pain. Other times a cutout underneath the big toe joint might create more motion. Most cases of orthotics for hallux limitus require trial and error.
- Shoe modification- the best shoes for hallux limitus are low heeled shoes with a rigid sole. The more rigid the sole, the less the big toe is called upon to try and bend.
- Modification of activities- in severe cases the avoidance of certain activities may go a long way to reducing the symptoms.
- exercises for hallux limitus- in spite of the fact that too much exercise can aggravate the big toe joint, physical therapy, where the joint is exercised and various modalities are used to reduce inflammation, may be of benefit, however, this benefit is usually short lived.
Surgical options
When conservative measures have failed and the pain is great enough then the patient should consider surgical intervention. Like most medical conditions, not all hallux limitus is the same. Things that have to be addressed are underlying causes of the condition; the type of gait the patient exhibits, the amount of bony overgrowth, the amount of joint destruction, the type of activity the patient would like to resume, the limited or lack of joint motion and of course the amount of pain.
|
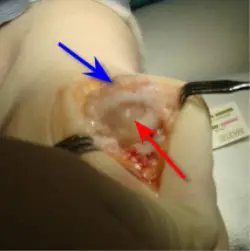
Joint remodeling Many times a patient can get by with just a remodeling of the joint meaning all the bony overgrowth is removed which should allow for better motion without pain. This is known as a cheilectomy. If you look at the picture above, the blue arrow reveals the bony overgrowth, while the red arrow reveals the head of the metatarsal bone. A normal metatarsal head should be pearly white. The metatarsal head in this picture has degenerative changes within it, indicative of osteoarthritis.
Osteotomy- Sometimes a wedge of bone will be removed from the top of the first metatarsal in an effort to allow the big toe to bend upwards over the metatarsal. This is known as a re-angulation osteotomy (surgical cutting and realigning of bone) which will allow better toe dorsiflexion (toe bending upward).
In these instances the source of pathology is the fact that the first metatarsal bone is not properly aligned with the big toe. The first metatarsal, instead of being even with the big toe, is actually elevated. This elevation is problematic because it does not allow the big toe to bend upwards over the first metatarsal bone and thus creates a jamming effect which worsens over the years.
Joint destructive procedure or Inplant- If the cartilage is destroyed, many times a joint destructive bunionectomy will be performed or a joint implant will be inserted. The problem with joint implants is that they eventually wear out and so relatively young active adults are not good candidates, because the more active an individual is, the quicker the implant will fail. Implants also increase the chance of complications and can be a real issue in cases of infection because the implant must be removed and now there is a large gap where the implant sat, that must be addressed.
First metatarsal phalangeal joint fusion- If the joint is too far gone and cannot be salvaged the joint may actually have to be surgically fused. Although there are situations where this cannot be avoided I personally do not like the procedure. Once the joint is fused, although there may no longer be pain in the joint, this procedure will change the individuals gait and that can lead to pain elsewhere, as well as reduction of certain activities.
REFERENCES
American College of Foot and Ankle Surgeons
continue with hallux limitus (surgical procedures)


Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…