psoriasis
AUTHOR: Marc Mitnick DPMREVIEWED BY: Podiatric Medical Review Board
home --> psoriasis
WHAT IS PSORIASIS
This is mainly a skin condition marked by patches of thick, red skin covered with silvery scales that occur primarily on your elbows, knees, legs, lower back, scalp and feet. Certainly not life-threatening, the condition can be painful, affect your ability to function, and cause psychological and emotional distress. Approximately one third of patients with this condition have a family history of the disease.
This type of eczema affects two to three percent of the Caucasian population which includes over seven million Americans with an estimated 125 million world-wide suffering from this affliction. This condition is seen less in African-Americans along with Asian and Eskimo populations. It is virtually unheard of in Native Americans. This condition is seen more in northern exposures as opposed to southern altitudes where people have greater sun exposure.
This dermatitis develops when the ordinary life cycle of skin cells accelerates. Skin cells regularly die and flake off in scales — but in people with psoriasis this process happens within days rather than weeks. Rounded, circumscribed, red, dry, scaly patches of varying sizes characterize the skin. Itching and burning may also be present. On removal of the scaling skin bleeding points occur known as Auspitz’ sign. Koebners’s phenomenon is also frequently found. This is the appearance of typical psoriatic lesions at the site of an injury.
types of psoriasis
- seborrheic which is the most common form.
- Inverse, seen more commonly in overweight people characterized by smooth patches of red, inflamed skin. Friction and perspiration cause it to worsen.
- Guttate, which primarily affects people under the age of 30 and is generally caused by a bacterial infection.
- Pustular, is very common on the feet but overall is rare. It occurs quickly, forming pus filled blisters which will dry out rapidly but then quickly reappear. When it occurs all over the body it can produce fever and chills.
- Erythrodermic, is the least common form which may be triggered by sunburn or medication. This can cover the whole body with a red peeling rash.
- Psoriatic arthritis, in addition to the skin reaction the joints may also be affected in the same way that arthritis affects the joints. Symptoms range from mild to severe. It may lead to permanent deformity but generally speaking is not as severe as other forms of arthritis .
The disease is chronic, but you may have periods when the condition becomes worse alternating with times when it improves or goes into remission. And although no cure exists, treatments may offer significant relief.
factors predisposing you to psoriasis
Aside from a positive family history being a risk factor for psoriatic conditions, other factors include stress which can have a negative impact on your immune system. Medications particularly beta blockers can predispose someone to this condition. Even lithium may make you more prone to pustular eruptions. Excessive exposure to sun can exacerbate the eczema, while small amounts of exposure to the sun may actually help the condition. People with HIV and children with frequent recurring infections may also be more prone to this type of eczema.
Below is a picture of a typical psoriatic eruption on the bottom of the feet.
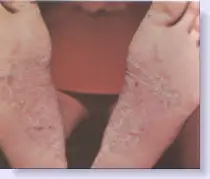
|
About 50 percent of patients with psoriatic eczema eventually develop the condition in the nails of the hands and feet. The classic changes seen within the nails is pitting of the nail plate. This is the result of damage directly to the nail matrix (growth plate of the nail). Other nail changes commonly seen in psoriatic nails include yellow discoloration of the nail plate along with detachment and crumbling of the nail and the accumulation of thick tissue under the nail. These nails may appear very similar to mycotic (fungus) nails.
Below is a picture of a psoriatic nail.
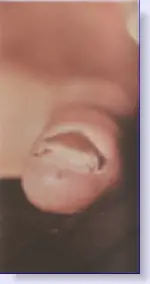
|
psoriatic arthritis
This is another aspect of this disease state that commonly manifests itself in the feet. Approximately 5-7 percent of those suffering from psoriasis will eventually develop arthritis. Men and women are affected equally. The peak incidence is in the fourth to sixth decade.
There are no specific laboratory findings in psoriatic arthritis so the condition has to be differentiated from other arthritides such as osteoarthritis, rheumatoid arthritis, and goutl . When a patient presents with the cutaneous manifestation of psoriasis the diagnosis is easy; it is more perplexing when there are no cutaneous or nail lesions (and no history of the actual disease).
Clinically in the foot psoriatic arthritis has certain characteristics. One is diffuse swelling of one or more toes commonly known as “sausage digits”. This is thought to be due to a combination of swelling from both arthritis and tenosynovitis.
Note the "sausage" appearance of some of the toes.
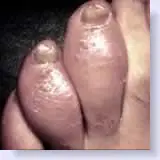
|
Although there are a number of skeletal manifestations of the disease the picture below notes the classic findings of psoriatic arthritis in the foot. The blue arrow points to a normal even joint space between the second metatarsal bone and the second toe. Notice the red arrow; that is a classic “cup and saucer” effect of the fourth metatarsal bone being jammed into the base of the fourth toe. The yellow circle shows the destruction in the toes that is characteristic of the disease. This destruction has occurred on the other toes as well.
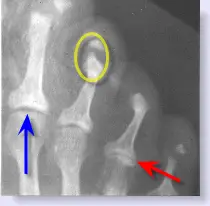
|
TREATMENT OF PSORIASIS
topical medications for psoriasis
Treatment for psoriasis is geared to reduce inflammation both in skin and bone manifestations. Since statistically most people who suffer from psoriasis suffer primarily skin eruptions topical medication is usually the treatment of choice.
- Hydrocortisone cream has always been the old standby. These creams not only cause an immune suppression but they are also anti-inflammatory. Chronic use of topical cortisone cream will have a tendency to thin out your skin. Another problem with cortisone cream is a condition known as tachyphylaxis, this is a situation where the patient has been using a topical cortisone cream for some time and all of a sudden it stops working. The patient may then try another topical steroid cream which initially will be beneficial, but then it too stops working. This can be very frustrating for the patient and the treating doctor. For this reason if you should start in with another doctor for your psoriasis, it is very important that you let he or she know what medications you have previously tried.
- Anthralin is a topical prescription medication that when properly used may send your psoriasis into remission for upwards of six months. It is messy to use and may stain clothing.
- Vitamin D Analogs may be used alone or in combination with topical cortisone creams. The vitamin D analog helps decrease inflammation and reduce plaque appearance. Tachyphylaxis does not appear to be a problem with this medication. Used in combination with a topical cortisone cream, it will reduce the side effects of the steroid cream. One such medication is Dovonex. It works by slowing down skin cell turnaround time which prevents formation of skin patches. Other medications in this class include Vectical, Galderma and Taclonex.
- Coal-tar ointments have been used for psoriasis for ages; they are sold over the counter in 1-5 percent strength. They are generally inexpensive but they are also greasy, messy to use, have an odor and are staining. They may also cause sensitivity to sunlight. A prescription item, Scytera foam was developed to decrease the greasiness and odor of traditional tar preparations. Coal tar preparations traditionally reduce inflammation and pruritus (itching).
- Tazorac is another medication, which seems to prolong psoriasis remissions. It is particularly helpful when used with moisturizers and ultraviolet light therapy. This medication is a synthetic retinoid that has an anti-inflammatory component. The drawback to this medication is that it can be extremely irritating to the skin. Since this medication needs to be applied directly to the psoriatic plaques, it can be helpful to apply vaseling on the healthy skin to avoid irritation. Another trick is to start using the medication every other day until it becomes tolerated.
- Keratolytics include urea, salicylic acid and lactic acid creams. These medications help remove excessive scaling. It may be used in conjunction with topical cortisone cream; the idea being that it enhances the penetration of the cortisone cream. But, with greater absorption comes the potential for more complications. These medications may also be used on psoriatic nails in an effort to thin them out.
- Moisturizers include over the counter emollients like Eucerin or Curel cream or even prescription emollients. They work by restoring the function of the epidermal (skin) barrier, decreasing water loss and improving the appearance of the skin. These emollients are best applied immediately after a bath or shower as they are better absorbed on moist skin. They too, may be used in conjunction with topical cortisone cream.
other treatments for psoriasis
- Ultra violet light has been used with success in psoriasis treatment as either ultraviolet B phototherapy or a photochemotherapy using ultraviolet light in combination with systemic or topical psoralen, which is a natural occurring compound that enhances the effects of the ultra violet light treatment. One can either soak in a solution containing psoralen or apply a topical cream containing psoralen and then have the ultra violet therapy.
- If you prefer to try some alternative treatments licorice root and chamomile are herbs that both contain anti-inflammatory compounds. Applied topically to the lesions may reduce the skin inflammation. Aloe cream has been shown to be effective.
- Since high protein diets are associated with an increase in inflammation through the body, reducing your consumption of protein rich foods primarily meat and dairy products may reduce flare-ups.
- Fish oil supplements are also known to have an anti-inflammatory effect on the body and therefore may reduce the inflammation of psoriasis. Four to six capsules a day containing EPA and DHA are recommended.
- For those with psoriasis, sunbathing can also be helpful. In a world where everyone is avoiding the sun out of fear of developing skin cancer, the sun’s rays have been shown to have significant therapeutic benefits. Psoriatic patches are far less common in most individuals during the summer months.
oral medications for psoriasis
- For psoriatic arthritis the simplest oral medication is the class of anti-inflammatory medication. This class of medication is reserved for moderate pain associated with the arthritic component of psoriasis. Click here for a recent warning issued by the FDA on anti-inflammatory medication (December 2006).
- In patients with more destructive disease the class of drugs known as DMARDS (disease modifying anti-rheumatic drugs) should be initiated. The most common drug in this class is Methotrexate, (a chemotherapy drug), which has been shown to be effective for both the cutaneous and articular forms of psoriasis.
- Anti-malarials also in this classification has been shown to be of help for both severe cutaneous and articular forms of psoriasis.
Additional drugs in this class include Sulfasalazine, Cyclosporin A, Etanercept, Remicade and Humira.
It is important to emphasize that these are serious medications and should not be abused.
See related article......eczema
See related article......nail fungus
REFERENCES
Centers for Disease Control and Prevention
Want more information? CLICK HERE


Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…