idiopathic toe walking
AUTHOR: Marc Mitnick DPMREVIEWED BY: Podiatric Medical Review Board
home --> toe walking
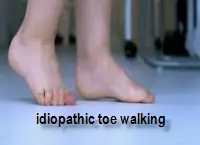
walking on toes with no associated neurological disease state
WHAT IS TOE WALKING
Idiopathic toe walking is a condition where a person, generally a child, walks on their toes in the absence of any disease state. Most young children begin walking around 12 months of age and it is not uncommon for many of them to walk on their toes during their initial period of learning to walk as they develop their gait pattern. If this pattern of walking persists beyond two years of age, it should be a cause for concern for parents and the condition needs to be investigated.
|
If all possible neurological disease states are eliminated and there is no history of trauma to the foot or leg, then a diagnosis of idiopathic toe walking is made. However, recently the thought process has become one where even in these cases, there may be a neurological component. Preliminary studies have shown a correlation between sensitivity to vibration and hypersensitivity in the feet as a reason for children to toe walk. This is an area that needs further investigation.
TREATMENT FOR TOE WALKING
After ruling out a neurological basis for this condition, idiopathic toe walking can be treated by a number of means and in combination.
Stretching exercises- children who walk on their toes show a tendency to exhibit a tight gastrocnemius and soleus muscles which are the two muscles below the back of the knee that come together and form the Achilles tendon. The younger the child, the more effective stretching exercises become.

|
Serial casting- is another avenue used to decrease the tightness of the Achilles tendon and associated muscles. A non-removable cast is applied to the foot to just below the knee. Each cast is left on for a period of time, determined by the physician. As a new cast is applied, the foot/feet is further dorsiflexed (bent upwards) in an effort to stretch the Achilles tendon and muscle group. This has to be done in stages as it would be very painful to the child and probably impossible to stretch the muscle group by trying to accomplish all the stretching necessary in the initial casting.
|
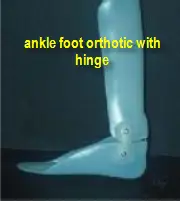
Night splint- In conjunction with an ankle foot orthosis, the child may also wear a night splint. This is a removable cast like device that is worn while the child sleeps and just like all the other treatment options attempts to stretch the achilles tendon.
Surgery- In more severe cases surgical lengthening of the Achilles tendon is employed. If the posterior leg muscle group is too tight and has not responded to the previous mentioned conservative options, then actually lengthening the tight heel cord may be the only means to allow the child to walk normally.
Botox- In recent years Botox injections have been employed with a mixed degree of success. Botox or botulinum toxin injections have the ability to relax muscle, so in theory if a child has a tight heel cord, injecting the muscle with Botox should loosen up the muscle. The injection in conjunction with night splints and stretching has had some degree of success.
It is worth noting that even with what may be considered a "successful" treatment, most children will require some kind of orthotic device going forward. In many instances, improvement seen with treatment degrades over time. Continued walking on the toes into adulthood can impact the quality of life as it is an altered gait and opens the adult for a myriad of problems.
REFERENCE
Lower Extremity Review, August 12, 2012, Volume 4, page 39
REFERENCES


Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…