ankle sprain
AUTHOR: Marc Mitnick DPM home --> ankle sprainLATERAL ANKLE SPRAIN
An acute ankle sprain is one of the most common injuries to present to an Emergency Room. Although an injury of this nature may occur on either the inside or outside of the ankle, the lateral ankle sprain (outside) is far more common. This type of injury can be a very troubling problem and if not properly treated may result in chronic pain.
This article will discuss treatment for simple sprains as well as more complex ankle injuries. Some of you who will be reading this are apparently having issues with this type of injury that has not gotten better. Hopefully you will learn the process that is involved in the treatment of more severe sprains to the ankle.
The vast majority of people who sustain this type of injury do not seek medical attention and those that do, in many instances are under treated. Once a patient is seen in the Emergency Room they are generally discharged and told to see a podiatrist or orthopedist for follow-up care; many people do not bother. If there is not proper follow-up this increases the chances of problems going forward. If initial treatment is not aggressive enough this can lead to an instability in the ankle joint and in some cases may require surgical intervention down the road.
The ankle joint is known as a hinged synovial joint meaning the motion of the ankle is limited to an up-down motion also known as dorsiflexion and plantarflexion. Any movement of the foot to the inside (inversion) or the outside (eversion) comes primarily from the subtalar joint which is just below the ankle joint.
The most common form of injury is known as a lateral ankle sprain or inversion sprain. This is where the foot bends inward below the ankle joint. This causes a severe stretching on the outside of the ankle and conversely a jamming effect on the inside of the ankle. An ankle sprain is considered by many doctors to be a partial dislocation of the ankle joint.
SEVERITY OF ANKLE SPRAINS
Ankle sprains are "graded" according to severity.
- Grade 1 is a minor strain with no tearing of ligaments.
- Grade 2 is a partial tear of the lateral ankle ligaments.
- Grade 3 is a full tear of one of the ligaments and possibly even a tear of what is known as the peroneal muscles that run directly underneath the outside of the ankle. Interestingly enough, sometimes a total tear of the lateral ankle ligaments can be less painful than a partial tear and this keeps the patient from seeking medical attention.
|
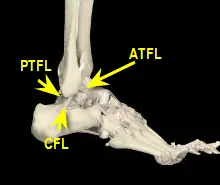
There are three ligaments that make up the lateral ankle ligaments. (ATFL) Anterior talo-fibular ligament. (CFL) Calcaneal fibular ligament. (PTFL) Posterior talo-fibular ligament. A partial tear of two of the ligaments may end up more problematic than just a complete tear of one ligament.
Most, if not all lateral ankle sprains initially may not be too painful, but as the day progresses, so does the pain and swelling. In addition to pain and swelling there may be eccymosis (black and blue) in the surrounding area. This just represents broken blood vessels and is not an indicator of the severity of the injury. When we as foot specialists examine someone who has sustained an inversion sprain, we examine both the outside and inside of the ankle, the alignment of the foot relative to the ankle, as well as the tendons that surround the ankle.
A fairly common occurrence with severe inversion ankle sprains is possible fracture of the fifth metatarsal base. During the injury, when the foot bends inward, it puts a lot of pressure on the outside of the foot and in many instances can actually fracture part of the fifth metatarsal bone. Many non-footspecialists will not look for this potential problem and a fracture of the fifth metatarsal bone may go undiagnosed.
Additionally, the motion available in the ankle has to be tested as well as the fibula bone along its course. The fibula bone is the long bone on the outside of the leg that forms the outside of the ankle joint. The longer the patient has waited to seek medical attention, the more painful and swollen the ankle will be, making it more difficult for the doctor to adequately examine all parts of the foot, ankle and lower leg that may be involved.
DIAGNOSING ANKLE SPRAINS
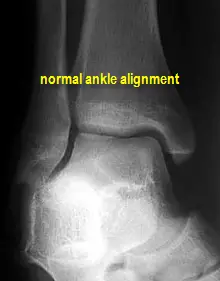
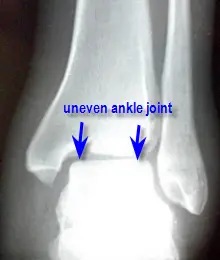
Once presenting to the doctor or an Emergency Room, x-rays will be taken. X-rays cannot visualize ligaments or tendons for possible damage, but they are taken to rule out fracture, either to the ankle itself, the fifth metatarsal bone or to the lower leg. It is important to note, that very small "cracks" in bone may not show up initially on x-ray, but if the patient does not respond in the appropriate period of time for an ankle sprain, additional x-rays or even an MRI may have to be considered to look for small fractures. X-rays on the initial exam are also helpful in recognizing abnormal joint alignment as a result of the sustained trauma. If there is a mal-alignment of the ankle joint with no fracture, casting may be required to re-align the ankle joint, otherwise, the patient may have chronic pain in the ankle. Sometimes surgery is also necessary if the ankle cannot be re-aligned through manual means.
|
|
The last thing we are looking for with radiographs is an osteochondral defect. What happens here is a piece of bone is chipped off the talus bone, which is the bone in the foot that is basically the bottom portion of the ankle joint. If one is found, in most cases it must be removed surgically. If left alone it can act as an irritant in the joint and thus a source of ongoing pain.
In the majority of cases initial x-rays will be negative for any bone pathology. Due to the expense involved, an MRI is usually not performed on initial treatment (unless a fracture is suspected and not seen on x-ray). Some institutions may consider doing a diagnostic ultrasound to check the integrity of the ligaments and tendons surrounding the ankle. This is an inexpensive and quick test.
TREATMENT FOR ANKLE SPRAIN
The treatment protocol for ankle sprains has changed dramatically over the last decade. Years ago the treatment of choice was rigid immobilization. This meant putting on a cast with the foot in proper alignment to the leg in order to allow the ankle to heal over time. Experience has shown that over immobilization, particularly in Grade 1 and Grade 2 sprains may lead to scar formation in the healing ligaments and tendons and can leave the patient with chronic pain. The only time a cast becomes mandatory is if there is an associated fracture with the ligament damage, or quite simply, the patient cannot bear weight on the foot. The use of crutches and remaining non-weightbearing on the foot would also be introduced at this time.
The alternative to a rigid cast would then be a soft supportive cast to help keep the swelling down, which will reduce pain, and to bear weight as tolerated. Within a few days, the soft cast may be replaced with an Aircast or other more mobile type brace which will allow the patient to start range of motion exercises in the ankle joint (as tolerated) in an effort to reduce scarring and maintaining motion in the ankle joint.
physical therapy for ankle sprains
In Grade 2 and Grade 3 sprains after about one week, the patient may want to start on a regimen of physical therapy. The purpose of which is to help facilitate the healing process, reduce edema, pain and increase motion in the joint, thus getting the patient healed quicker.
Grade 1 ankle sprains are treated a little bit different. Most of you are familiar with R.I.C.E. (Rest, Ice, Compression, Elevation). This along with anti-inflammatory medication (assuming you can tolerate them) is all that is necessary. Within a few days the ankle should feel better and each day should bring further improvement.
In an otherwise healthy individual Grade 1 ankle sprains take about one month to resolve themselves. A Grade 2 sprain in most cases will take upwards of two months and sometimes slightly longer while a Grade 3 sprain may take upwards of six months to fully resolve. This is not to say that you will not be walking, but more than likely you will need to ambulate with some form of ankle support, women in particular, will not be able to wear certain types of shoes and both men and women will have to refrain from certain athletic activities.
SHOULD I USE ICE OR HEAT FOR LATERAL ANKLE SPRAIN?
There is the ongoing debate of whether ice or heat is better for injuries such as a sprained ankle. Various doctors have different opinions. My feeling is that ice is necessary for the first 24 hours, simply to reduce swelling which will reduce pain. Cold clamps down blood vessels and reduces the amount of blood flow to an area and in this instance will then reduce swelling. The problem is that blood flow to an area is the way the body heals all types of injuries. It does so by bringing nutrients to the traumatized area. After 24 hours, when the swelling (and pain) have stabilized, it is time to discontinue ice and switch over to heat. Generally moist heat works better than heat from a device like a heating pad. By applying heat to the area, the blood vessels in the area dilate (open up) and more blood is able to flow into the area and begin the healing process.
CHRONIC ANKLE SPRAIN
In general, if you reach a point where you are not seeing further improvement each week and you are still having difficulty walking then it is time for further investigation. The guidelines given above are not carved in stone. If progress is not being made each and every week, particularly if you are having physical therapy, then a re-evaluation is necessary.
At this point an MRI would be indicated as this test will show damage to soft tissue meaning ligament, tendon and muscle. An MRI may also show a fracture that was not visible on x-ray. An osteochondral lesion (defect in bone from trauma) may also be visible. It is important to correlate any abnormal findings to the area where the patient is experiencing pain, as an MRI may show old injuries which are not part of the present problem.
SURGICAL TREATMENT OF ANKLE SPRAINS
In cases where the ATFL (anterior talo-fibular ligament) and the CFL (calcaneal fibular ligament) are both torn, this may require surgical intervention to repair the ligaments as a tear in two ligaments may be creating an instability in the ankle joint and thus continued pain. (See diagram) The third lateral ankle ligament is the PTFL (posterior talo-fibular ligament). A tear of just the ATFL generally does not have to be repaired as one tear in most cases will not cause ankle instability. The most common procedure done for lateral ankle tears is the Brostrom procedure which is a primary repair of the torn ligaments using suture anchored into the fibula bone. This will be followed by casting for as long as six weeks, but some authorities are now suggesting casting for as little as three weeks and then physical therapy, again, in an effort to create better motion in the joint. It should be pointed out, that by nature of the procedure, there will be some limitation of motion following this procedure. This occurs because the post-surgical ligaments are tighter than the pre-trauma ligaments.
Other surgical procedures done may require repair of the peroneal tendon on the outside of the ankle and if it determined that there indeed is an osteochondral defect, then that piece of bone may have to removed as well, usually via ankle arthroscopy.
MEDIAL ANKLE SPRAINS
Eversion ankle sprains as the name implies, are sprains on the inside of the ankle. This is a far less frequent injury then lateral ankle sprains because the mechanism of injury is far less common. This type of injury will occur primarily in athletes because they find themselves in awkward foot positions when doing their sport, along with being off balance many times. This type of injury is usually due to an eversion type of injury where the foot bends outward from the ankle (the exact opposite of an inversion sprain). Examples that might cause eversion sprains include a gymnast who continually misses a "landing" and the foot bends outward, or perhaps a soccer player who is running up and down a field that is all "beat up" causing the foot to over stretch and rotate outwards.
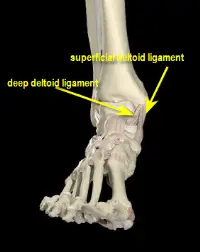
In addition to eversion injuries being less common than inversion injuries the ligament on the inside of ankle, known as the deltoid ligament is a much stronger ligament than the lateral ankle ligaments. Actually, there is a superficial and deep deltoid ligament and therefore is stronger than any of the lateral ankle ligaments singularly.
|
When making a diagnosis of medial ankle sprain the mechanism of injury is important to know. This will alert your doctor to look at the inside of the ankle, as well as the outside. Unfortunately in most sporting events the injury is a result of a collision and all the athlete remembers is ending up on the ground.
The treatment for a medial ankle sprain is basically the same as already discussed for lateral ankle sprains. Initially x-rays will be taken to rule out fracture and to view the ankle morTise (the alignment of the ankle itself). Examination of the posterior tibial tendon is necessary as they pass just inferior to the inside of the ankle joint. These tendons have a greater propensity to "stretch" than to tear. Immobilization with an early return to weight bearing as tolerated by the patient is the standard course of therapy and once again should the patient not heal in an acceptable period of time further studies such as an MRI may be needed.
One difference in medial ankle sprains versus lateral ankle sprains is the use of orthotics. Orthotics nave the tendency to invert the foot and in doing so will reduce the strain on the deltoid ligament. This should make walking more comfortable and the healing process quicker. On the outside of the ankle an orthotic will cause a stretching of the soft tissue structures and this of course can exacerbate the problem of lateral ankle sprains.
RESUMING ATHLETIC ACTIVITY
The question always asked by athletes is when can they return to their activity. This is not an easy question to answer. Due to the complexity of ankle sprains as previously described, there is no cookie-cutter rule. The biggest concern is returning to athletic activity too soon and re-injuring the ankle, possibly worse than the original injury. Depending on age, weight and overall health, many people will experience chronic tenderness in an ankle that is clinically healed, particularly those individuals who have sustained repeated ankle sprains.
In my practice, when I feel a patient is clinically healed I first have them put the ankle to the "test" to make sure it will hold up to the rigors of their sport. I have them do some light running and other mobility exercises. Their response will allow me to give them advice going forward. Some will return to their normal activities in no time, while others will be forced to reduce their athletic activity and even have to use some sort of mobility brace just to stabilize the ankle with the expectation that over time the ankle will further improve.
REFERENCES
Want more information? CLICK HERE


Recent Articles
-
Vitamin D impact on health
Feb 06, 23 07:17 PM
Researchers are suggesting that the effectiveness of Vitamin D in fighting and preventing disease is predicated on a persons body mass index (BMI). The thinner the person the greater the positive impa… -
Foods to speed up healing
Feb 01, 23 02:41 PM
One of the best ways to help yourself heal faster after surgery is to eat well. Getting the proper nutrition will provide your body with the essentials it needs to promote healing. Here is a suggestio… -
Cancer and Type 2 Diabetes
Jan 25, 23 04:52 PM
An article revealing that older type 2 diabetics have a higher incidence of cancer then non-diabetics. It is suggested that cancer may surpass CVD as the number one cause of death in older diabetics. -
Does glucosamine or MSM reduce arthritis pain?
Jan 22, 23 01:41 PM
A good review of the possible benefits to taking glucosamine, chondroitin or MSM for arthritis. Always beware of the possible side effects of over the counter supplements. -
shin splints
Jan 18, 23 05:12 PM
A great review on the various causes of shin splints, along with treatment options. -
Whats new in skin cancer?
Jan 15, 23 08:32 PM
A presentation of newer skin protection combinations in an effort to better protect the skin from the hazards of sun exposure. -
Causes and risk factors of warts
Jan 14, 23 05:02 PM
A good review of the causes of warts and protective measures you can take to prevent developing them. -
Do chronic wounds need to be dressed daily?
Jan 11, 23 02:18 PM
Because of supply chain shortages as well as staffing shortages particularly during the pandemic, many institutions extended the time between dressing changes for chronic wounds. Is this really the be… -
Food choices that raise your risk of type 2 diabetes
Jan 08, 23 10:07 AM
A good review of how blood sugars can become elevated and the harm that can do. Certain food groups have a tendency to raise your blood sugars and should be avoided. -
Outcome stats from Scarf bunionectomy
Jan 03, 23 03:04 PM
The Journal of Foot and Ankle Surgery recently reported a meta analysis of outcomes in 1583 Scarf bunionectomies that met their inclusion criteria. Adverse events did not seem to be any better or wors…